Powerful
Lessons

A strong focus on service learning empowers students and
faculty to improve health and change the world

By
Pam Auchmutey


Each
year, migrant workers follow the harvests up the East Coast in search
of work. Many come to the farms near Moultrie, Georgia, to pick fruits,
vegetables, and tobacco and
to sort and package produce for market.

The
difference between ‘service’ and ‘service learning’
is that
the latter must be something the community wants and values.
— Dr. Judith Wold, 81MN
Visiting Scholar and
Interim Director of the
Office of Service Learning


Emory
nursing senior Susie Kahl
prepares to take a student’s blood pressure.


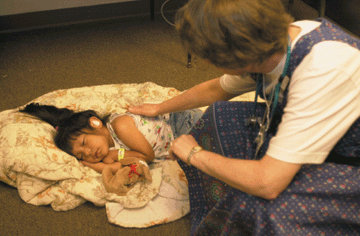
Students
and faculty (top photo) set up
tables and equipment for screening and assessing farm workers near
the community of Little Mexico.
Students (bottom photo)
do intake for families who arrive
at the clinic site that evening.


Lilabet
Choate, 97N, 02MSN (L–R, top photo), speaks with a farm worker through
interpreter Myrna Alejandra Ramiro. Emory nursing senior Joseph Smith
(bottom photo) checks the hemoglobin and
glucose counts for a young man.


The
Migrant Family Health Program helps
relieve aches and pains for workers like these young men, who stoop and
lift constantly and quickly to pick bell peppers on a farm near Moultrie,
Georgia. The more buckets they fill, the more money they earn.

I
was hoping to come away with a little more knowledge. I came away with
the world.
— Rebecca Berrier Lowrey, MSN03
South Georgia Migrant Health Project Participant

Lilabet
Choate, 97N, 02MSN, will never know what happened to the quiet, soft-eyed
Mexican girl she examined last summer in southwest Georgia.
The 3-year-old was among those who had come to the gymnasium at Sunset
Elementary School in Moultrie, where a friendly army of health volunteers
was screening students enrolled in a summer program for the children of
migrant farm workers.
The toddler’s symptoms told the story—fever, a dry cough, a
crackling sound in her right lung, a rapid heart rate, and a breathing
rate of 40 respirations per minute, twice the normal number. It was clear
to Choate that the little girl had pneumonia.
When the child’s concerned father arrived, Choate urged him to take
his daughter to a pediatrician or emergency room for further assessment
and treatment. “Will she be able to go to school tomorrow?”
he asked in Spanish. “No,” Choate told him through an interpreter.
“Your daughter is very ill and needs to stay home from school.”
Now a graduate of the family nurse practitioner program at Emory, Choate
is fairly sure her young patient was back in school the next day. “We
weren’t able to find out,” she says, “but we felt certain
that she did not go to the hospital.”
As health professionals who work with migrant populations well know, families
often postpone seeking medical treatment because they can’t afford
to lose wages by missing work. This reality hit home for Emory and other
Atlanta-area nursing and health sciences students who took part last June
in the Migrant Family Health Program. For nearly a decade, the program
has been a valuable resource for farm workers who settle in Colquitt,
Tift, and Cook counties each summer to pick and pack fruits, vegetables,
and tobacco. Established by the Georgia State University (GSU) School
of Nursing in 1994, the program offers health screening, health education,
and episodic care to farm workers and their children. Last year, the Nell
Hodgson Woodruff School of Nursing became the lead organization in the
program after it moved from GSU to Emory.
“It’s the best thing I’ve done in my undergraduate and
graduate experience,” says Choate, who is also a cardiac nurse clinician.
“It pulls everything you know together.”
A real-world classroom
For two hot, hectic weeks, Choate and her fellow students plunged into
a real-world classroom to practice their clinical and evaluation skills,
think on their feet, collaborate with others, and expand their social
awareness. They saw their share of common ailments—ear infections,
lice, vision problems, aching joints and muscles, foot infections, skin
rashes, anemia, hypertension, high blood sugar—and more serious cases—a
woman suffering an anxiety attack, a young man with an irregular heart
beat—which they referred to the local clinic.
Collaboration was also the norm. Together, nursing students and faculty
from Emory and Kennesaw State universities, dental hygiene students and
faculty from Clayton State College and University, and physical therapy
and psychology students and faculty from GSU saw just over 1,000 people,
almost half of them children.
Mornings began at Sunset Elementary, where various students led children
through health, developmental, and psychological evaluations. Family nurse
practitioner students gave physical exams and referred those needing further
treatment to local health facilities. Dental hygiene students provided
the youngsters with fluoride treatments and sealants. In the process,
each child’s school health record was updated.
During the evening, students and faculty set up shop at a different work
camp or packing shed to render health care and education to adults. Each
afternoon, Emory students attended a seminar on a topic related to migrant
health, while one or two students accompanied a county outreach worker
to deliver medicine to families and instruct them on how to use it. Some
students also ventured into the fields to observe crops being harvested,
sorted, and packed for shipping—something most had never seen.
To say the least, the Migrant Family Health Program is “an intensive
immersion learning experience” for both students and faculty, says
Lorine Spencer, the nursing consultant who leads the program she first
directed at GSU.
 |
| Judith Lupo Wold, 81MN, has been part of the Migrant Family Health Program since its beginning. |
A
new umbrella
At Emory, the program is part of the nursing school’s new Office
of Service Learning (OSL), designed to integrate the values of service
and
social responsibility more fully with the nursing curriculum, student
development, and community-based research. It also enables the school
to expand its work locally and globally through partnerships that address
health disparities and the health needs of vulnerable populations.
“Service learning has been part of the School of Nursing forever,
but not in an official capacity,” explains Dr. Judith Lupo Wold,
81MN, a visiting scholar from GSU who serves as interim director of the
OSL. “Several projects existed informally through various faculty
for a long time. It made perfect sense to incorporate them more formally,
especially since service learning is part of our mission from the highest
levels of the university on down.”
The OSL is the umbrella for several projects, including migrant health.
For the second year in a row, family nurse midwifery students shared their
knowledge and skills with the South Georgia Migrant Health Project, led
by the Physician Assistant Program in the Emory School of Medicine. This
program serves another 1,000 adults and children in different counties
in southwest Georgia.
Back in Atlanta, nursing students and faculty care for senior adults at
Williamsburg Clinic, screen and counsel homeless men at Café 458,
and educate and mentor health sciences students at Booker T. Washington
High School. New service learning projects are pending, such as an immunization
initiative for children in Cuba and a cancer education program for underserved
populations in Georgia.
A promising gift
These projects earned impressive points for the School of Nursing last
fall, when The Helene Fuld Health Trust made a five-year, $5 million commitment
to social responsibility through service learning. The largest gift ever
to the school supports a scholarship endowment for the Emory Nursing Segue
Program, which targets second-career students who want to make a difference
in the world. Each recipient will study an area of social concern in nursing
and will receive a bachelor’s and a master’s degree in nursing
after three years of study (see “Nurturing
Social Responsibility” in the "New Developments" Section).
“This unprecedented gift holds tremendous promise for us,” says
Dean Marla Salmon, whose own career is grounded in serving others through
public health and health policy. “Each Fuld Fellow is required to
participate in an area of service learning to help correct health disparities
and make a positive impact on social policy.”
And although service projects have been a part of university life for
quite a while, the School of Nursing is among the few in the nation to
create an office dedicated specifically to service learning.
“If universities were ivory towers, they certainly cannot afford
to be now,” says Emory University President William Chace. “The
great universities of the next century will be those that put not only
their brains but also their hearts into meeting the world’s needs.
In that respect, the Office of Service Learning is an important component
of Emory’s long-standing mission to improve human well-being.”
Like their students, nursing faculty benefit as the OSL assists them in
creating new projects for learning and identifying new opportunities for
research that will help improve the community. “Most nurses have
done lots of service in their careers—perhaps not with students,
but service nonetheless,” says Wold. “The difference between
‘service’ and ‘service learning’ is that the latter
must be something the community wants and values.”
 |
| Cynthia Hernandez is one of many community leaders in Colquitt County who help make the Migrant Family Health Program a success. She directs the county’s Farm Worker Health Program at the Ellenton Clinic. |
Rooted
in community
The Migrant Family Health Program is a prime example.
Beyond students and faculty, it touches the lives of many others—migrant
workers and their children, the farmers for whom they work, the state
and county agencies that assist them, local churches that serve meals
to students and faculty, Georgia businesses that donate toiletries and
other items to make goody bags for migrant families, and community members
who volunteer translation and other services.
Among
them is Cynthia Hernandez, who winces inwardly if she hears someone complain
about the high cost of produce. “Paying $1.79 for a pound of tomatoes
may seem high to someone else but not to the farmers who make sure that
produce gets to your table,” says Hernandez, director of the Colquitt
County Farm Worker Health Program at the Ellenton Clinic. “Every
day is a gamble.”
The same is true for migrant farm workers, whom Hernandez and others assist.
A typical day may find the workers in a field of bell peppers, earning
35 cents for each bucket they pick. Young men in their 20s stoop constantly
to fill their buckets. Once filled, the men hoist their bucket to their
shoulders and run to empty it at a trailer parked in the field. There
the men toss up their buckets to another worker, who empties them. Another
worker, a woman, places a fichas (chip) in each empty bucket and
hands it back to a worker, who rushes to fill it all over again. At the
end of the day, the workers turn in their chips to be paid. They also
earn their share of aches and pains. Fortunately, relief is not far way.
By early evening, the health sciences students and faculty from Atlanta
have set up tables and supplies in the front yard of a small, white frame
house that serves as a Hispanic church for residents living in a cluster
of mobile homes known as Little Mexico. The church provides much-needed
electricity for the Nightingale van, a mobile clinic on loan from South
Georgia College. Outside the van, nursing students from Emory and Kennesaw
staff tables set up for checking in and screening the farm workers. Nursing
faculty aboard the Nightingale van examine men and women who need more
thorough evaluation for conditions such as pregnancy, breathing problems,
heart ailments, and sexually transmitted diseases. Students from GSU and
Clayton State staff separate tents that offer physical therapy and dental
care.
On this particular night, Emory nursing senior Sarah Cohan is doing intake
with the help of an interpreter. Although Cohan speaks Spanish, she is
glad the interpreter is there to help her follow what each person is saying.
“The interpreters who volunteered from the community were awesome,”
Cohan recalls later. “They went above and beyond the call of duty,
helping us set up and take down our gear. Some of the things we discussed
with patients were not always pleasant. But the interpreters were very
professional in dealing with these types of issues. They made the farm
workers and their families comfortable and were key to the whole operation.”
Like Cohan, Choate relied on an interpreter to figure out why a young
man’s right eye was so irritated. She soon determined that he was
suffering from pterygium, the result of countless hours in the sun. With
time, the tissue growing in the inner corner of his eye would cover it
completely, blinding him. Although his condition is treatable with surgery,
Choate instructs him, it will recur unless he protects his eyes by trading
his ball cap for a sombrero. He should also consider working inside a
packing shed instead of picking crops outdoors. “If you lose your
vision, you won’t be able to work,” she tells him through her
interpreter.
For the most part, the health problems that Choate and her colleagues
see are less sobering but require care nonetheless. Year after year, cavities
rank as the No. 1 problem among both adults and children. This fact keeps
the dental hygiene students jumping to assist dentist Heather Watkins,
who is extracting teeth by lamplight in a mesh tent. The first dentist
to volunteer with the Migrant Family Health Program, Watkins offers a
much-needed service, since migrant families lack access to regular dental
care.
Emory nursing senior Menaka Ponnambalam watches the dentist at work from
outside the makeshift dental office, which resembles a MASH unit. “The
integrity of the care here is no less than what patients receive in a
doctor’s office or hospital,” says Ponnambalam. “That’s
why so many people flock to us for dental and medical care. They’re
very appreciative of what we do.”
Profound changes
Several miles away in another county, the family nurse midwifery students
witness something quite similar as they team with Emory physician assistant
students to assess and treat patients. “The experience was a real
eye-opener regarding how migrant families live, their priorities in terms
of their health and work, and the conditions in which the students provide
health care,” notes Dr. Marcia McDonnell, 77MN, assistant professor
(clinical) of nursing.
Like their counterparts near Moultrie, these students assessed and screened
schoolchildren during the day. At night, they cared for adults with elevated
blood pressures, heart block, diabetes or depression; pregnant women;
and infants with ear infections.
“We all worked together in helping each other learn,” says Kathryn
Matthews, associate (clinical), who supervised the family nurse midwifery
students with McDonnell. “Everyone was on equal footing.”
Caring for those families had a profound effect on their students. “Before
the trip, I was scared to death,” confesses Rebecca Berrier Lowrey,
MSN03. “I was afraid I would be so lost, but I wasn’t. I was
hoping to come away with a little more knowledge. I came away with the
world.”
 |
Each summer, the Migrant Family Health Program screens and treats approximately 1,000 adults and children in rural southwest Georgia. Rooted in the community, the program has strong alliances with academic institutions, agencies, businesses, individuals, and local organizations. Partners include the Colquitt County and Georgia Department of Human Resources migrant health programs; the Clayton State College and University Dental Hygiene Program; Georgia State University’s physical therapy and psychology programs; Kennesaw State University School of Nursing; South Georgia College; the Colquitt County health and labor departments, medical center, and extension service; the Southeastern Primary Care Consortium/Atlanta Area Health Education Center; the Southwest Georgia Area Health Education Consortium; and local groups and individuals (farm owners and workers, physicians, churches, businesses, the US Marine Corps, and volunteers). Through these partnerships, Emory’s School of Nursing helps care for some of the 100,000 migrant laborers who work Georgia’s crops each year.