











|
 |
 |
Simulating stent placement
Post-stent:keeping arteries open in diabetes
Highest honors
Metabolic syndrome and stress
Mapping an anti-cancer molecule
How estrogen prevents bone loss
Radiation robots |
Fear factor
A new day and a new chair of pediatrics
Creating an anti-reflux barrier
Controlling seizures deep within the brain
New leader of radiology |
 |
| |
|
|
 |



Simulating stent placement
The
Food and Drug Administration (FDA) recently approved a new technique
for treating potentially life-threatening blockages in the arteries
of the neck that lead to the brain. The carotid stenting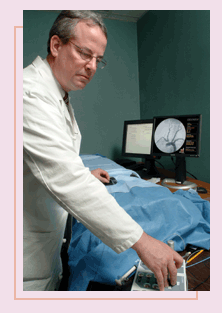 procedure offers a minimally invasive alternative to carotid endarterectomy
in patients with carotid artery disease who are at risk for stroke.
procedure offers a minimally invasive alternative to carotid endarterectomy
in patients with carotid artery disease who are at risk for stroke.
The procedure has fewer bad outcomes
compared with carotid endarterectomy, according to Emory Heart
Center cardiologist Christopher Cates.
FDA approval of the Guidant carotid
stent and embolic protection system (the latter, a tiny filter to
catch clots stirred up by the procedure before they float to the
brain) will allow treatment of patients with blocked carotid arteries
who have been unable to undergo surgery due to lung disease, heart
disease, or other illnesses. However, the FDA recommends that physicians
who use the carotid stenting device undergo special training.
Working with the Society of Cardiovascular
Angiography and Interventions, the Emory Heart Center is one of
30 training sites for carotid stenting across the nation and one
of the first to develop a training program using virtual reality
simulators. With the simulators, which look like human mannequins,
physicians practice threading a catheter through an artificial circulatory
system as they view angiograms of the “patient’s”
heart.
“For the first time, physicians
are able to practice on simulators,” says Cates. “Just
as airline pilots learn to fly on simulators, physicians can practice
on simulators before performing carotid artery stenting on patients.”
|
 |
| |

TOP


|
 |
 |
 |
Post-stent:
keeping arteries open in diabetes
Following
angioplasty, stents are frequently used to keep newly widened arteries
open. However, renarrowing, or restenosis, is a frequent problem,
especially in diabetic patients. A multi-center study, led
by Emory cardiologist John Douglas has found that restenosis
in diabetics undergoing coronary stenting can be reduced significantly
with the drug cilostazol. The CREST (Cilostazol for RESTenosis)
trial found a statistically significant decrease in restenosis
in diabetic patients receiving cilostazol over placebo. This
benefit persisted even in a group of diabetic patients with
smaller vessel sizes, the most challenging population to achieve
durable results with stenting.
stents are frequently used to keep newly widened arteries
open. However, renarrowing, or restenosis, is a frequent problem,
especially in diabetic patients. A multi-center study, led
by Emory cardiologist John Douglas has found that restenosis
in diabetics undergoing coronary stenting can be reduced significantly
with the drug cilostazol. The CREST (Cilostazol for RESTenosis)
trial found a statistically significant decrease in restenosis
in diabetic patients receiving cilostazol over placebo. This
benefit persisted even in a group of diabetic patients with
smaller vessel sizes, the most challenging population to achieve
durable results with stenting.
|
 |
|
 |
| |

TOP


|
 |
 |
 |
 |
Highest
honors
The
Institute of Medicine (IOM) has elected four Emory faculty
to its new class of leading national health scientists: Mahlon
DeLong (neurology), Stephen Warren (human genetics), Ricardo
Martinez (emergency medicine), and Ruth Berkelman (Rollins
School of Public Health). In addition, the IOM elected two
adjunct Emory faculty members: CDC Director Julie Gerberding
and James Marks, also of CDC. Whereas a decade ago, Emory
had only one member in the IOM, today it boasts 20 in the
institute. Membership represents one of the highest honors
in medicine.
|
 |
|
 |
 |

TOP


|
 |
 |
Metabolic syndrome and stress
Could autonomic
dysfunction, signaled by changes in heart rate variability, play
a role in the development of metabolic syndrome? Could this explain
an increased coronary artery disease mortality risk in persons with
metabolic syndrome? Emory research suggests that’s the case.
 The
American Heart Association estimates that approximately 47 million
U.S. adults now have metabolic syndrome, a nearly five-fold increase
in the past 40 years. People with the syndrome display a combination
of symptoms that include increased abdominal fat, obesity, high
blood sugar, raised levels of triglycerides, and low levels of HDL.
A key underlying abnormality in metabolic syndrome is insulin resistance. The
American Heart Association estimates that approximately 47 million
U.S. adults now have metabolic syndrome, a nearly five-fold increase
in the past 40 years. People with the syndrome display a combination
of symptoms that include increased abdominal fat, obesity, high
blood sugar, raised levels of triglycerides, and low levels of HDL.
A key underlying abnormality in metabolic syndrome is insulin resistance.
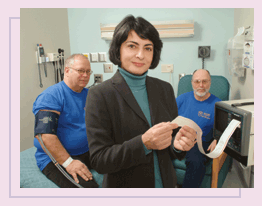
An Emory research team, headed by
Viola Vaccarino, examined whether autonomic dysfunction
(as measured by heart rate variability) is associated with insulin
resistance. Among the participants (160 middle-aged male twins free
of symptomatic coronary artery disease), those with greater insulin
resistance had lower heart-rate variability scores. The association
was unchanged with adjustments for age, education, and smoking behavior.
While the actual causes of metabolic
syndrome remain uncertain, data are accumulating to suggest that
autonomic and neuroendocrine abnormalities typical of the stress
response may play a role. “Our findings fit into this picture,”
says Vaccarino. “If the role of stress in everyday life and
its impact on metabolism is clarified, this may have a huge impact
on our understanding of what causes metabolic syndrome as well as
help us to better prevent diabetes and heart disease.” |
 |
 |

TOP


|
 |
 |
Mapping an anticancer molecule
Emory
scientists, collaborating with researchers
at three national laboratories, have solved the structural puzzle
of how an emerging class of cancer drugs work to halt cell division.
The findings may lead to the creation of more effective cancer treatments.
“Uncovering and mapping the structure of this model system
will assist scientists around the world in creating new compounds
that could lead to new cancer drugs, says Jim Snyder, an Emory chemist
and director of biostructural research.
Published in Science, the
report includes the first 3D, atomic-scale images of the binding
site where one of the drugs, epothilone A, interacts with a key
protein controlling cell division. The researchers have examined
two drug families—the epothilones and taxanes. The drugs work
to halt the division of cancer cells by binding to the same site
on a protein called tubulin that is involved in cell division.
Jim Nettles, an Emory doctoral candidate in molecular and systems
pharmacology and first author on the paper, hopes that the model
system will be useful as a clinical tool for matching the best drug
to a given patient. |
 |
| |

TOP


|
 |
 |
How estrogen prevents bone loss
SCIENTISTS HAVE UNCOVERED
a new link in the chain of immune system events through which estrogen
prevents bone loss. Through research in mice, scientists found that
an immune-signaling molecule called type b transforming growth factor
(TGFb) is responsible for a cascade of events that leads estrogen
to prevent bone loss. When TGFb signaling in T cells is blocked,
the bone-sparing effects of estrogen are lost.
Garland Herndon Professor of Medicine
and Director of the Division of Endocrinology Roberto Pacifici
and research associate Yuhao Gao led the study, published in Proceedings
of the National Academy of Sciences.
Pacifici and colleagues removed ovaries
from mice and then studied the effects of estrogen on immune cells
and on bone marrow in culture. They found that the level of TGFb
in the bone marrow macrophages of mice lacking ovaries was about
half that of mice with ovaries. When they treated the mice with
estrogen, levels of TGFb in the bone marrow increased about three-fold
in mice with ovaries and about eight-fold in mice without ovaries.
To test the effects of TGFb on bone-marrow
density, the scientists used a transgenic mouse model in which TGFb
signaling in T cells is blocked. Although these mice had the same
level of bone density as control mice at birth, they gradually lost
bone density over time, suggesting that when T cells are insensitive
to TGFb signaling, they stimulate the loss of bone. These findings
could lead to new therapeutic approaches for preventing bone loss. |
 |
 |
|
 |
 |
 |
Radiation
robots
Emory
is the first health care facility in the United States to
deliver new, ultra-precise radiotherapy treatments using a
fully robotic, on-board imaging system for tracking tumor
locations and positioning patients. The image-guided radiation
therapy uses a newly developed On-Board Imager and Clinac
linear accelerator from Varian Medical Systems. 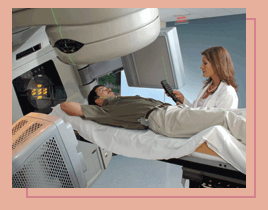 The
technology is expected to improve the precision and effectiveness
of cancer treatments by giving doctors the ability to accurately
track and adjust for tumor movements at the moment of treatment. The
technology is expected to improve the precision and effectiveness
of cancer treatments by giving doctors the ability to accurately
track and adjust for tumor movements at the moment of treatment.
With the precision of techniques
like image-guided radiation therapy, doctors can deliver higher
doses to the tumor while reducing the dose to nearby critical
structures, says Lawrence Davis, chair of Radiation Oncology,
“which can only translate into better tumor control
and fewer complications.”
The On-Board Imager is a digital
imaging system mounted on the treatment machine via robotically
controlled arms that operate along three axes of motion so
that they can be positioned optimally for the best possible
view of the tumor and surrounding anatomy. The device produces
high-resolution images of the tumor, and it also can track
tumor motion to provide doctors a clear indication of exactly
how a tumor will move during treatment due to normal breathing
and other physiologic processes.
|
 |
|
 |
 |
|
 |
 |
 |
FEAR
FACTOR 
Afraid
of heights? Emory scientists have found a potential cure.
In a study of 28 people suffering from acrophobia, study participants
received either a tuberculosis drug (D-cycloserine, or DCS)
or a placebo, followed by two virtual reality sessions that
simulated standing in a rising glass elevator. Compared with
subjects who took only placebo, those treated with DCS experienced
a significant reduction in their fear of heights that was
maintained for at least three months after concluding therapy.
The mechanisms governing the fear response, located in the
amygdala region of the brain, function abnormally in an acrophobic’s
brain. DCS binds to neurotransmitter receptors in the amygdala,
and when combined with virtual reality exposure therapy, DCS
facilitates fear extinction in the acrophobic’s brain.
The study, led by Michael Davis, Kerry Ressler, and Barbara
Rothbaum in Emory’s Department of Psychiatry and Behavioral
Sciences, appeared in the November issue
of Archives of General Psychiatry.
|
 |
|
 |
 |
|
|
 |
A new day and a new chair for pediatrics
Barbara
Stoll, an
internationally recognized pediatrician who specializes in issues of neonatal infectious
disease and child survival, has been named chair of the Department
of Pediatrics and medical director of Children’s Healthcare
of Atlanta at Egleston.
recognized pediatrician who specializes in issues of neonatal infectious
disease and child survival, has been named chair of the Department
of Pediatrics and medical director of Children’s Healthcare
of Atlanta at Egleston.
Stoll’s appointment to the newly
combined posts will further cement a strong leadership connection
between Emory and Children’s, which have enjoyed a long historical
association at their adjacent Clifton Road campuses. Many of the
doctors at Children’s at Egleston are Emory pediatrics department
faculty members.
Shortly after Stoll’s appointment,
Emory Children’s Center physicians moved from modular buildings
located behind Children’s at Egleston into a nearby, newly
constructed $42 million Emory Pediatrics Building. Children’s
at Egleston is launching a hospital expansion project on the 2.4
acres of land vacated by Emory upon the opening of the new pediatrics
center.
Stoll has been a faculty member at
Emory since 1986, serving as interim chair of the pediatrics department
for the past year, following the departure of former chairman Devn
Cornish. She also has been named to serve as president and CEO of
the Emory Children’s Center, the largest pediatric multispecialty
group practice in Georgia, and as president of the Emory Egleston
Children’s Research Center.
“This is a new day for pediatrics at Emory,” says Stoll.
“Our new building is a wonderful metaphor for a fresh and
invigorated department. There are challenges ahead, but for the
first time in the history of the Department of Pediatrics, we have
beautiful new space—consisting of both a wonderful pediatric
clinic and state-of-the-art, 21st century laboratories for scientific
research.”
Along with her appointment as chair, Stoll is the first holder of
the new George W. Brumley Jr. Chair in Pediatrics, supported by
a $2 million gift and pledge from the Zeist Foundation of Atlanta.
Brumley, who served as chair of pediatrics from 1981 to 1995, died
along with 11 family members in a tragic plane crash during a family
trip to Kenya in 2003.
“George Brumley was the man who hired me and one of my mentors.
There is a certain poignancy every time I think about holding a
chair that bears his name,” says Stoll. “He left big
shoes to fill, and I am humbled and honored to serve as the George
Brumley Chair.” |
 |
 |

TOP


|
 |
 |
 |
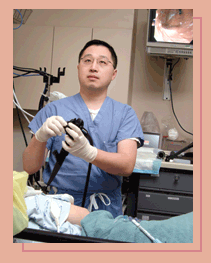
Creating an anti-reflux barrier
Gastrointestinal surgeons at Emory are among the first in
the world to treat patients suffering from gastroesophageal
reflux disease (GERD) with a simple, outpatient endoscopic
procedure that takes less than an hour. More than 15 million
Americans suffer from daily heartburn, one of the most common
symptoms of GERD.
 “Reflux
can be a very debilitating condition, and this procedure gives
patients a viable option to traditional surgery and costly
medications,” says Edward Lin, assistant
professor of surgery. “Reflux
can be a very debilitating condition, and this procedure gives
patients a viable option to traditional surgery and costly
medications,” says Edward Lin, assistant
professor of surgery.
The new procedure differs from
traditional surgery, in which part of the upper stomach is
wrapped around the esophagus to create a new anti-reflux valve
from the exterior of the gastroesophageal junction. The new
technique is a full suturing method that attempts to create
a “ball-valve” anti-reflux barrier from inside
the upper stomach relying completely on endoscopy.
The technique uses a device
consisting of a reusable instrument called a plicator, a single-use
cartridge containing a suture-based implant, and a specially
designed endoscopic tissue retractor. The device is passed
orally into the stomach over a guide wire and sutures the
inside of the stomach at the gastroesophageal junction to
tighten the valve, stop reflux, and restore the natural anti-reflux
barrier. Normally, a muscular valve at the end of the esophagus
keeps stomach contents from refluxing into the esophagus.
However, in GERD, this valve is weak or relaxes too frequently,
allowing stomach contents to flow freely into the esophagus.
“This is appropriate for
patients with complex conditions—especially for those
who cannot undergo more invasive surgery or who choose an
intermediate procedure between medications and surgery,”
says Lin. The procedure was approved by the FDA in April 2003.
|
 |
|
 |
 |

TOP


|
 |
 |
Controlling seizures deep within the brain
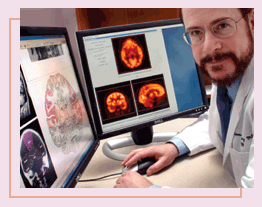 ABOUT
20% OF PATIENTS WITH EPILEPSY lack control of their disorder
because either anti-epileptic medications are ineffective or they
fail to qualify for standard epilepsy surgery, according to Emory
neurologist Thomas Henry. Emory is exploring two alternatives for
these patients: deep-brain stimulation therapy and vagus nerve stimulation
(VNS). ABOUT
20% OF PATIENTS WITH EPILEPSY lack control of their disorder
because either anti-epileptic medications are ineffective or they
fail to qualify for standard epilepsy surgery, according to Emory
neurologist Thomas Henry. Emory is exploring two alternatives for
these patients: deep-brain stimulation therapy and vagus nerve stimulation
(VNS).
Deep-brain stimulation has proved
effective for other neurologic conditions such as Parkinson’s
disease. In the SANTE trial (stimulation of the anterior nucleus
of the thalamus for epilepsy), researchers at Emory and 11 other
sites will study whether deep-brain stimulation of the thalamus
(one of the areas of the brain most involved in seizure circuitry
and development) will improve conditions for epileptics.
Under general anesthesia, participants will have a lead, or thin
wire electrode, implanted in the anterior nucleus of the thalamus
on both sides of the brain, which will be connected to a single
pacemaker-like device implanted under the skin near the collarbone.
The leads and pacemaker will then be connected by extension wires
threaded under the skin of the neck. The stimulation from the device
will deliver electrical pulses directly to the targeted areas in
the brain through the extension wires and leads.
 The
SANTE study is significant because it will enroll a larger number
of participants than previous pilot studies, and it will include
a longer study period, a total of 13 months. The
SANTE study is significant because it will enroll a larger number
of participants than previous pilot studies, and it will include
a longer study period, a total of 13 months.
Already Emory researchers have found
that VNS may activate areas of the brain for longer periods, up
to months or longer, than previously thought. VNS is the only FDA-approved,
implantable, electrical stimulation therapy for epilepsy. The scientists
measured neuronal activity before and after long-term VNS and found
a reduction in seizures when higher levels of VNS were used.
Using positron emission tomography,
the researchers found that cerebral blood flow changes showed increased
synaptic activity in the so-called “sensory strip” of
the brain’s cortex—an expected finding because the patient
felt mild sensations during stimulation. VNS also activated the
thalamus and other brain areas involved in memory, thinking, alertness,
arousal, and emotional processing. With higher levels of stimulation,
blood flow was increased more than at low stimulation in these areas.
“These findings show that cerebral
blood flow changes in various areas of the brain help in reducing
seizures when activated by VNS,” says Henry. “Some types
of seizures start in the thalamus, but this research suggests that
we may be able to control widespread seizures that begin in other
areas of the brain with VNS." |
 |
 |

TOP


|
 |
 |
New leader of radiology
 Sanjay
Saini, widely recognized for
applying his research expertise and business skills to developing
top-tier working environments in academic medicine, has been appointed
the William Patterson Timmie Professor and Chair of the Department
of Radiology and professor of radiology. He also holds a joint appointment
in the Goizueta Business School. Sanjay
Saini, widely recognized for
applying his research expertise and business skills to developing
top-tier working environments in academic medicine, has been appointed
the William Patterson Timmie Professor and Chair of the Department
of Radiology and professor of radiology. He also holds a joint appointment
in the Goizueta Business School.
A specialist in gastrointestinal radiology
and liver imaging, Saini previously served on the faculty of Harvard
Medical School for 23 years. He was director of Computed Tomography
at Massachusetts General Hospital and vice chair of radiology for
Health Systems Affairs. He also was director of Partners Radiology,
a collaborative organization encompassing five acute care systems.
Saini’s research interests included
clinical research and management investigation. His early clinical
research focused on developing novel contrast agents to improve
imaging of liver tumors. More recently, he has been examining work
flow of radiology departments, cost reduction, and improving quality
of care.
Saini succeeds William Casarella,
who continues as executive associate dean for clinical affairs in
the School of Medicine. Casarella, professor of radiology, is currently
focusing on Emory’s clinical services at Grady and also providing
clinical services in radiology.


|
 |
|
|
|





