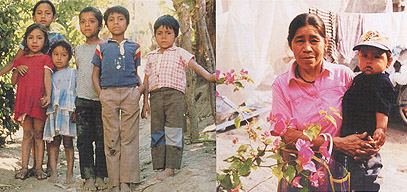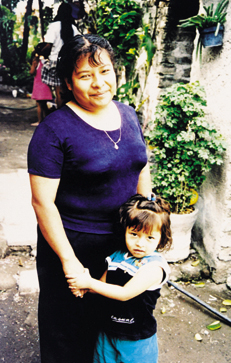The gaunt faces, distended bellies, and stick-like arms of severely malnourished children provoke an immediate, emotional response. When malnutrition is severe, the need for nutritional intervention is obvious. However, according to Woodruff Professor of International Nutrition Reynaldo Martorell, “these severe forms, with their dramatic clinical signs, are relatively rare, even in poor countries.” A more common problem––and one of more massive proportion—is that of mild and moderate malnutrition. In fact, this problem is so large that it reaches the level of international catastrophe. UNICEF even classifies mild and moderate malnutrition as a “silent emergency.” In South Central Asia, despite steady progress, underweight is still expected to be prevalent in 40% of the population in 2005. In sub-Saharan Africa, child underweight is predicted to rise to 38% by that year. Regional pockets in Latin America hide levels of malnutrition similar to those of the sub-Saharan African countries. In a Distinguished Faculty Lecture at Emory University, Martorell outlined some of consequences of poor nutrition, which extend well beyond childhood. Early malnutrition accounts for pronounced growth failure in very young children who remain stunted as adults. Maternal stunting increases the risk of fetal malnutrition, thereby transmitting the problem across the generations. Additionally, malnutrition may impact intellectual performance and even have an effect on an adult’s economic potential.
In April, Martorell received the SINR/Kellogg Prize for International Nutrition, which recognizes excellent research in the field. While he cites overwhelming evidence that economic investments in education and control of infectious disease more than pay for themselves, “the evidence that nutrition leads to significant economic returns remains weak,” he says. The Rollins School of Public Health has set out to change that with a host of studies that are quantifying the power of early childhood nutrition on human potential. In research that stretches from Latin America to Europe, RSPH investigators are exploring the link between nutrition and economic productivity, between famine and adult chronic health problems, and between micronutrient supplementation and birth weights. Some of these studies rely on a specific nutritional intervention while others focus on food fortification or economic incentive programs.
In it for the long haul By necessity, then, nutrition trials need to span years to glean accurate information. And often, positive results don’t appear right away. For example, in Honduras, international health professor Rafael Flores is two years into a nutrition intervention to reduce stunting, but so far he has been unable to demonstrate any impact. After 27 months of an ongoing study in Mexico, another faculty member, Usha Ramakrishnan, has yet to find any improvements in birth size from a multivitamin-mineral supplement given to pregnant women.
But as Martorell has learned, initially disappointing results can lead to surprising findings years later. He participated in a nutrition intervention in Guatemala that concluded in 1977 that was able to show beyond a doubt that consumption of a nutritious drink called atole reduced low birth weight, cut infant mortality, and improved child growth. However, researchers working on the study––conducted by the Institute of Nutrition in Central America and Panama (INCAP)––were disappointed because they were unable to show a link between improved nutrition and cognitive development. Despite that disappointment, the INCAP study has now become one of the longest running and most fruitful nutrition trials in public health history. Its success became evident in a follow-up study led by Martorell in the 1980s. He found that the adolescents who had received atole as children showed marked intellectual improvement over their counterparts who had received a less nutritious drink called fresco. And, coupled with education, the effects of atole magnified as the years of schooling increased.
Currently, Martorell has a $1.5 million grant from the National Institutes of Health to take the work even further, investigating the link between early childhood nutrition and economic productivity. Of 2,393 subjects in the original 1977 study, his team has been able to locate and include 1,558 people—or close to 72%––in this second follow-up. Whereas his first follow-up demonstrated the educational and economic potential of these subjects, this study is gauging actual productivity of a population that has now reached adulthood. The researchers are completing physical exams of the subjects and their spouses, drawing blood samples, taking blood pressure, and measuring height, weight, and body composition. To measure educational achievement, they are administering a battery of tests on general knowledge, mathematics, reading, comprehension, and vocabulary. Colleagues at the International Food Policy Research Institute in Washington, D.C., and the Department of Economics at the University of Pennsylvania are collaborating on the economic analysis. “The assessment of economic productivity in rural areas is no easy task,” says Martorell, “because often there is no payment or paycheck involved. Part of the household may plant corn or beans, and they consume some and sell some.” Analysis of the data will begin in one year, when Martorell hopes that study will reap a harvest of findings that policy makers can’t ignore.
She is now following the growth and development of 400-500 children aged 3 months to 2 years, who are the children of the women in the pregnancy study. These children are enrolled in either a control group that receives vitamin A and iron supplements or a treatment group that is given a daily multivitamin-mineral supplement. Previous research has examined the impact of a single nutrient, but Ramakrishnan wants to gauge the effect of an array of micronutrients on child development. Later this year she hopes to add omega fatty acids to her list of supplements. Her goal, like others on the faculty in international health, is to get results that in turn inform policies and support programs that improve child health.
Stein has worked with this population for more than 10 years, studying first the reproductive outcomes of women exposed to famine during gestation and now the effect of famine exposure on cardiovascular risk. Together with colleagues at Columbia University and Leiden University Medical Center and the Dutch Institute for Public Health, he is focusing on people who were either born after the famine started or conceived before it ended, a cohort now in their late 50s. The researchers, supported by an NIH grant, hope to determine whether starvation during pregnancy, particularly during the first trimester, has any impact on adult health. They are enrolling approximately 1,500 participants, a task made possible because Holland maintains population registries and has well-kept records going back 60 years. Specifically, Stein wants to know if the long-term effects of famine can be modified. “Through a strong study design, we hope to show that in this case of a known nutritional insult that nothing is happening during pregnancy to trigger chronic health conditions,” he says. “We hope to differentiate between the independent role of early life and adult lifestyle.” To account for social factors that may have affected fecundity during the famine, the investigators are evaluating the health of not only the children affected by the Dutch Famine but also one of their same-sex siblings. They will obtain a range of body measurements, administer diet and physical activity questionnaires, collect a history of major clinical events, and survey adult risk behaviors such as smoking as well as screen for cardiac conditions and glucose tolerance. “The short-term effects of famine are well-known,” says Stein, “but the long-term effects aren’t.” And it is the long-term effects that may affect preventive health care and policy decisions the most.
He is running similar trials in Nicaragua and Honduras, which are being closely watched by government leaders who want to set effective deterrents to stunting in their own countries. “These are large social experiments in developing countries, and they will have tremendous implications for policy,” says Flores. In convincing policy makers to invest in nutrition, Martorell argues that “such an investment contributes to building human capital and for this reason should be considered a long-term economic strategy.” Feed the child, and you develop a stronger and smarter adult, one in turn capable of building a stronger and smarter society. Another compelling reason is that adequate health and nutrition are basic human rights. “What is the goal of development if not to satisfy basic human needs?” Martorell asks. “Is it not the role of responsible government to provide for at least the bare minimum for human well-being?”
Yet in a world where large disparities exist between rich and poor, where gaps between nutrition and malnutrition are growing, how can researchers most effectively influence the process? One way, says Ramakrishnan, is through training and dissemination of information. In collaboration with the Centers for Disease Control and Prevention, she is leading the design of a digitally based training program in nutrition for regional professionals who are involved through industry or government in some aspect of micronutrient nutrition worldwide. The program will cover basic information on global nutritional status, as well as nuts-and-bolts training on how to assess, survey, and evaluate local nutrition projects. Another strategy is to allocate financial support where it is most needed. In India, for example, where the rate of child underweight approaches 50%, there is no need for more research to document the problem, says Ramakrishnan. Instead money is needed for program support to increase birth weights among those with low weights–a difficult proposition for funding agencies used to spending money on surveying and evaluating rather than doing. Perhaps the best way is gathering the hard data to inform effective policy. RSPH is adding to that scientific database with a host of studies that are quantifying the power of early childhood nutrition: Martorell’s linkages between nutrition and economic productivity in Guatemala; Flores’ interventions on stunting in Honduras, Nicaragua, and Brazil; Stein’s exploration of famine’s effect on chronic health; Ramakrishnan’s examination of low birth weights in Mexico; and other faculty efforts to fortify flours or to establish universal salt iodization. These investigators are rallying together for a common cause, to maximize human growth and potential-to insure a fruitfil legacy.
This News Could Save Your Life | An idea, of SORTS | Class Notes Rollins School of Public Health
Copyright © Emory University, 2003. All Rights
Reserved. |