|
 |
|
|













|

|
|
|
| |
Highlights: |
|
|
| |
Almost
ready for prime time
Water for the world
Lowance center offers new immunity deal
Fundraising report: How we did in FY '04
New
faces in high places
|
|
Women
test new gel to fight HIV
Computer screening saves lives
Milestones
Targeting hard-to-treat tumors |
 |
| |
Almost
ready for prime time
By
Pam Auchmutey
The
second phase of the Emory Electronic Medical Record (EeMR)
will soon go live with a cast of thousands, as more than 7,000 physicians,
nurses, pharmacists, therapists, nutritionists, unit clerks, schedulers,
administrative staff, and others begin using the new software applications
that will support it.
Phase II is a major milestone for
EeMR, a 10-year, $50 million project that will transform care delivery
throughout the Emory Healthcare (EHC) system. In 2002, Phase I included
the installation of the system’s technical infrastructure
and hardware, as well as the Enterprise Master Patient Index, software
that tracks each patient using a unique internal identifier number.
This index reduces registration errors and eliminates the need to
re-enter the same patient information in different care settings
and is also used for PACS, the radiology picture archival and communications
system used to store and display medical images electronically.
Rollout of the new programs in two-week
phases began in late January, starting at Wesley Woods Hospital,
then moving to Emory Crawford Long Hospital, followed by Emory University
Hospital. The Emory Clinic began gradually implementing the programs,
a section at a time, in February. Most users are receiving two hours
of classroom instruction beforehand, while physicians are being
trained individually.
“The size of this is incredible
to me,” says Anne Nelson, director of organizational development
and learning services for EHC. Nelson is the team leader responsible
for planning educational content. Implementation of Phase II required
the scheduling of nearly 900 separate training classes.
EHC employees can rest assured that
the instruction will not end there. As the software programs go
live, 500 ACEs—employees trained as Application Content Experts—will
be available during each shift to answer questions and troubleshoot
problems.
During Phase II, EeMR’s designers
will launch updated versions of existing software, including PowerChart
(inpatient results), PowerOrders (a physician/clinician order management
system), PharmNet (hospital-based pharmacy), and Charge Services
(hospital billing). New applications include PowerChart Office (an
outpatient version of PowerChart) and CV Net (a scheduling system
for hospital cardiology services). Emory University Hospital also
will go live with FirstNet (emergency department tracking and documentation),
which has been in use at Crawford Long since 2002, when it was installed
as part of Phase I. Cerner Corporation, a longtime EHC partner,
is providing the software.
All of these foundation applications
will support Phase III, the point when total transformation of patient
encounters will begin. The integrated information systems will lead to a
safer health care environment, administrators say.
will lead to a
safer health care environment, administrators say.
Slated to begin in 2006, Phase III
will include new technology and processes such as computer-based
physician order entry (CPOE), which will enable hospital and clinic
physicians to enter orders in a computer terminal in or near exam
rooms and at the patient bedside.
Not only will CPOE help eliminate
imprecise and incomplete communication among doctors, nurses, and
pharmacists, but it will also provide real-time decision support
to help reduce adverse drug events and other errors. Organizations
such as the Leapfrog Group and the Institute of Medicine advocate
using CPOE to minimize medical errors, the fourth leading cause
of death in the United States.
“The transition will be challenging—not
just learning the new technology but using it as a tool to change
our processes so that we can do our work more effectively and safely,”
says William Bornstein, chief quality officer and medical director,
information services, for EHC. “The real payback will be improvement
in the quality, safety, and satisfaction of all involved—our
clinicians and our patients. Those are the major goals.”
In addition to charting clinical data,
EeMR will capture and document insurance information and other data,
thus eliminating the manual paperwork that occupies a great deal
of doctors’ and nurses’ time.
“We’re not looking for
this system to provide help with the brilliant stuff,” says
Bornstein, who is an adviser to Leapfrog. “Those are the things
only our providers can do. But it can off-load tasks that can be
distracting—things like multiple documentation requirements
and managed care formularies—and leave more time for the deep
thinking that is required for high-quality patient care, more time
for physicians to focus on the patient.”
For now, EHC staff and patients will
live in a hybrid world of paper and electronic records. The use
of paper will diminish as use of the electronic record grows—a
transition projected to last until 2012. Ultimately, every patient
and EHC worker will feel the impact of EeMR.
“This is the biggest challenge
our organization has ever had,” says Kate Smith, EeMR project
director. “It’s going to affect everybody in our health
care system.”
Pam
Auchmutey is senior associate director of Health Sciences Publications,
and the editor of Emory Nursing magazine.
|
|
 |
| |
|
|
|
| |
| |
Water
for the world
By
Diane Blanks
Today,
it is estimated that nearly 2 billion people worldwide lack access to safe drinking water, and
more than 1 million people die each year of water-transmitted diseases.
2 billion people worldwide lack access to safe drinking water, and
more than 1 million people die each year of water-transmitted diseases.
Retired public health professor
Eugene Gangarosa, who has devoted much of his career to safe-water
projects, hopes a recent gift to the Rollins School of Public Health
(RSPH) will help change those dire statistics. Gangarosa and his
wife, Rose, have pledged $2 million to establish the Eugene J. Gangarosa
Chair in Global Safe Water and made a planned gift of another $2
million to establish the Rose Salamone Gangarosa Chair in Environmental
Health, a position focusing on improving sanitation in the developing
world.
“United Nations Secretary-General
Kofi Annan has pinned the world’s hope for global development
and stability on access to fresh water and sanitation,” Gangarosa
notes.
The problem is not that the world
doesn’t understand the causes of waterborne illness, he believes,
but that many approaches have not included practical “point-of-use”
strategies to improve access to cleanwater at the individual level.
In many areas of the world, simple,
low-tech, low-cost solutions can make a major difference, Gangarosa
says. For example, many families without running water must travel
long distances to communal wells. But the water, often carried in
open containers, is contaminated during transport back to the home.
During the 1980s, however, the Centers
for Disease Control and Prevention developed a special, narrow-mouth,
20-liter jug that enabled users to treat water with chlorine at
the source and then safely transport it. In countries that field-tested
the jugs, incidence of waterborne diseases was reduced by 50%. The
system is now in use in countries throughout the developing world.
 Gangarosa
began his public health career in 1959 as one of the first doctors
working on the international fight against cholera. At the time,
data from the World Health Organization indicated that waterborne
diseases annually killed almost 5 million people. Gangarosa
began his public health career in 1959 as one of the first doctors
working on the international fight against cholera. At the time,
data from the World Health Organization indicated that waterborne
diseases annually killed almost 5 million people.
Now, thanks to the development of
effective medical treatment, the mortality
for cholera is almost zero, but getting treatment and prevention
efforts to those who need it is still a worldwide challenge.
A medical doctor with a master’s
degree in microbiology, Gangarosa has worked around the globe in
a number of different roles. But the issue of safe water was never
far from his mind.
The couple also has funded a safe-water
endowment at the CDC through the CDC Foundation and established
a family foundation that contributes to a number of international
safe-water initiatives.
With their current gifts, the Gangarosas
hope to encourage future public health leaders to continue to find
practical but innovative ways to address this global emergency.
Their efforts to foster global safe
water and sanitation are, Gangarosa says, “drops of water
in an ocean of need,” but ones that they hope will grow and
expand over time.
Diane
Blanks is an editor in Health Sciences Development.
|
|
 |
| |
|
|
|
|
| |
Lowance
center offers new immunity deal
Why
do some healthy 40-year-olds have immune systems that look like that of
an 80-year-old? And how does this influence their risk of developing
cancer, heart disease, or Alzheimer’s later in life?
healthy 40-year-olds have immune systems that look like that of
an 80-year-old? And how does this influence their risk of developing
cancer, heart disease, or Alzheimer’s later in life?
These are some of the questions under the microscope at the new
Kathleen B. and Mason I. Lowance Center for Human Immunology at
the School of Medicine. Married scientists Cornelia Weyand and Jörg
Goronzy, who collaborate on research in this area, recently moved
from the Mayo Clinic to Emory to lead the effort.
The multidisciplinary center, which
opened in May, is dedicated to improving treatment of autoimmune
diseases and researching the ways that the immune system influences
development of chronic disease.
“We are seeing a paradigm shift
in modern medicine,” says Weyand, the first David C. Lowance
Chair in Human Immunology at Emory. “Traditionally, medicine
has been organized around organ systems. But it’s become increasingly
clear that diseases in many different organs share common principles
of how tissue functions fail. Medical specialties of the future
will center on such common biologic pathways.”
The best example, right now, is cancer
research and treatment that focus more on how cells in general turn
malignant, and less on the specific organ systems involved.
“The same will eventually be
true of many other diseases,” she says.
Scientists are just beginning to understand
the role that the immune system, in particular the inflammatory
response, plays in diseases not previously considered immune-related.
Although most people think of it as the body’s primary defense
against infection, changes in the immune system actually cause or
exacerbate many medical conditions.
“For instance, the inflammatory
response prompted by the buildup of plaque in coronary arteries
promotes the life-threatening blockages or tears that we associate
with heart attacks,” Weyand explains.
“The immune system causes disease
when it fails to protect us against cancer and infections and, equally
important, by driving inflammation, which we are beginning to realize,
is pivotal not only in rheumatologic and allergic diseases but in
other chronic diseases as well,” adds Goronzy, the new Mason
I. Lowance Chair in Human Immunology. “We must develop the
tools to measure the functionality of the immune system in those
who are healthy and in those who become sick when the system fails.”
“The body’s immune response
capabilities change throughout a person’s life and diminish
significantly after age 40,” Weyand explains. The new center
will study the ways that aging affects immune system function and
examine the role inflammation plays in the development of heart
disease.
“The center will also serve
as a force for integrating immunology research with existing medical
disciplines and helping Emory chart the course for modern medicine
in the 21st century,” Goronzy adds.
“In the future, medical research
will look very different from today, and the leadership at Emory
is active in guiding and shaping this process,” he explains.
“Recognizing genetic and environmental risk factors and developing
the instruments, such as bioinformatics, to quantify complex processes
will be key for the delivery of high-quality health care and for
disease prevention. Diseases do not adhere to our current specialty
designations, and they don’t read medical textbooks. Every
leading medical center will need integrated platforms to share information
along new clinical pathways.”
| |
|
|
| |
Grateful
patients offer ongoing tribute
Mason
I. Lowance, who graduated from Emory University School of
Medicine in 1927, practiced allergy and internal medicine
for 50 years. Among his notable patients were Goodrich White,
former president of Emory, and Atlanta mayors William B. Hartsfield
and Ivan Allen Jr.
When the highly respected allergist
retired in 1979, gifts from many of his grateful patients
and their friends provided seed money that eventually grew
into the $12 million endowment that now funds the Lowance
Center for Immunology and the Lowance chairs.
“My father was an allergist
when very little was known about the immune system,”
says David Lowance, a renal specialist for whom one of the
Lowance chairs is named. “We requested that the term
“immunology” describe the center to connote a
desire to elucidate and discover basic underlying mechanisms
of immune disorders, whether they be clinically expressed
as allergy, transplant rejection, cancer, rheumatoid arthritis,
or the many other diseases we now know to be related to disorders
of the immune system.”
|
|
 |
|
|
 |
| |
|
|
|
|
| |
|
|
|
|
|
|
| |
Fundraising
report: How we did in FY '04
The
Woodruff Health Sciences Center closed a banner year for
fund-raising in fiscal year 2004, raising just over $61 million
in total gifts to the schools of medicine, nursing, and public health,
the Yerkes National Primate Research Center, and Emory Hospitals.
“We continue to see substantial
giving from a growing list of donors who have faith in the work
we do in the health sciences,” says Phil Hills, Emory’s
vice president fordevelopment in the health sciences. “In
just the past five years, we have seen our annual totals go from
about $15 million to more than $61 million, excluding the Woodruff
Foundation gifts.”
Faculty have been important to this
success. Increased faculty involvement has allowed development professionals
to seek support from more sources for new programs and research
and has helped Emory better communicate its vision for making people
healthy, Hills says.
In 2004, fund-raisers were particularly
successful in securing endowment gifts to provide ongoing support
for education and research in medicine and public health. Last year,
a record 10 chairs and professorships in the health sciences were
endowed with gifts of $1 million or more, which will allow those
positions to receive continued support as endowment funds generate
their own income.
“Endowment gifts are particularly
important because they provide a stable source of income over time
to support the faculty in research, teaching, and patient care,”
Hills adds. “As we continue to see health care income diminish
due to declining reimbursements, this support will be more important
than ever.”
|
|
|
Gifts
of $1 million or more to the health sciences in fiscal 2004 included
the following:
Rollins Chair in Pain
Management
Mason Chair in Pediatric
Liver Transplantation
George Brumley Chair in
Pediatrics
Kamal Mansour Professorship in Surgery
Eugene J. Gangarosa Chair
in Global Safe Water
Rose Salamone Gangarosa
Chair in Environmental Health
Radiation Oncology
Professorship in Medical Physics
Radiation Oncology
Professorship in Cancer Biology
Michael and Laura Baur
Professorship in Orthopaedics
R. Harold Harrison Professorship in Orthopaedics
Avon Cancer Patient Navigation Program
Joe Craver Cardiothoracic
Surgery Fund
Mason Trust Gift to
Transplantation Clinic
AFLAC support to Pediatric
Building
Georgia Cancer Coalition
Patient Navigation Match
Glenn Family Breast Cancer
Equipment Research Fund
|
|
|
| |
|
|
 |
|
| |

|
|
In the Spotlight
The Emory Children’s
Center moved into a new home this winter. Construction of the $42
million facility was made possible by donations from the Woodruff
Foundation, AFLAC, the Francis Wood Wilson Foundation, and the Family
of the late George Brumley, a former chair of the department of
pediatrics, among others. |
|
 |
| |
|
|
|
| |
| |
New
faces in high places
This
year, the School of Medicine welcomed new leadership in
two key specialties: a veteran researcher and teacher in pediatrics
and an imaging specialist with an interest in improving work environments
as the new head of radiology.
In August, internationally recognized
pediatrician and neonatal researcher Barbara Stoll, a member of
the pediatric faculty since 1986, was named chair of the Department
of Pediatrics and medical director of Children’s Healthcare of
Atlanta at Egleston.
Pediatrics and medical director of Children’s Healthcare of
Atlanta at Egleston.
The joint appointment, which marks
the first time an Emory pediatrics chair has also been the medical
director at the hospital, will serve to further cement the close
relationship between the two institutions, Stoll says.
“In my mind, it is extremely
important that the Emory chair has a leadership role at Children’s,”
she adds. “It says that Emory is committed to Children’s
and that Children’s is committed to Emory. The relationship
is more than a collaboration—it is a partnership in every
sense of the word.”
In addition to the new position, Stoll
presided over the opening of a new $42 million, 153,000-square-foot
pediatrics building, featuring space for state-of-the-art research
laboratories and expanded room for clinical care and medical education.
“The new building represents
an extraordinary opportunity and also a responsibility,” Stoll
continues. “The first challenge is to fill our research laboratories
with creative, productive, cutting-edge investigators who will work
on important areas to prevent and treat
childhood disease.”
The department is also working to
design and implement the “ideal patient encounter,”
she adds. Woodruff Health Sciences Center CEO Michael Johns challenged
the department last year to develop a model for delivering the highest-quality
patient care and service to children and their families through
the Emory Children’s Center, its affiliated pediatric multispecialty
practice.
Across the Emory campus,
the Department of Radiology welcomed new chair and former Harvard
Medical School professor
Sanjay Saini.
Saini, a specialist in gastrointestinal
radiology and liver imaging, served on the Harvard faculty for 23
years, also holding concurrent positions
as head of computed tomography and vice chair of radiology for health
systems positions
as head of computed tomography and vice chair of radiology for health
systems
affairs at Massachusetts General Hospital.
Radiology is increasingly important
in the delivery of health care, Saini says. Where x-rays and CT
scans used to be used exclusively for diagnostic purposes, imaging
is now more integrated into health care delivery, with a wide array
of imaging services used to guide treatment.
The challenge for Emory and other
centers will be to find better ways to integrate radiology services
at the point of patient care.
“In the past, when we wanted an image,
we used to send the patient to radiology,” Saini says. “Now
we are moving toward having imaging technology at the bedside and
available immediately in the emergency room and other places.”
Another challenge will be to develop
efficient operational models that will allow such advanced imaging
technology, though it is very costly, to be available across the
entire Emory system to serve the largest number of patients.
“We don’t want to have
high-quality imaging just at Emory University Hospital or at the
clinic, but at Crawford Long and other facilities across our coverage
area,” he states.
Saini also holds a joint appointment
at the Goizueta Business School and hopes to focus some efforts
there on developing new models for efficient health care delivery.
“Emory already has a strong
tradition in radiology,” Saini says. “In this specialty,
traditional morphologic imaging is now being complemented by advances
in functional and molecular imaging. By delivering radiologic services
at the time of clinical care, radiologists are becoming increasingly
central to the practice of high-quality, cost-effective medicine.”
|
|
 |
| |
|
|
|
| |
| |
Women
test new gel to fight HIV
Believing
an HIV vaccine is still
years away from the market, many public health experts
are placing more emphasis on finding new treatments and technologies
to prevent the spread of infections.
One option, topical microbicide gels
that kill the virus on contact, may hold particular promise for
protecting women, says Frances H. Priddy, director of the Emory
Vaccine Center’s Hope Clinic in Decatur.
“Both biologically and socially,
women have been shown to be more vulnerable to infection with HIV,”
she says. “Due to some features of our anatomy, we are more
likely to contract the virus from male partners than they are from
us. And women in many cultures lack bargaining power in relationships
to negotiate condom use.”
The clinic recently received a five-year,
$2.2 million grant from the Centers for Disease Control and Prevention
to evaluate the safety and acceptability of the vaginal use of topical
microbicides in both healthy women and women already infected with
HIV. Recent research with primates has shown some topical agents
to be effective in preventing transmission of the simian form of
the virus.
Opened in 2001, the Hope Clinic is
a community-based, nonprofit research clinic dedicated to finding
new ways to prevent HIV and other diseases of global concern. Several
clinical trials of different HIV vaccines are currently under way
there. And in January, the clinic began enrolling volunteers in
a Phase 1 study of UC-781, an antiviral agent in the same category
as the AIDS drug nevirapine.
The early studies will focus on discovering
any side effects or adverse reactions the agents may cause, such
as rashes or irritation of the application site, and on the attitudes
of male partners of the women toward their use of the gel.
“Although we are not going
to test it on the partners and we don’t want them exposed
to it at this early stage, we do want to know what they think about
it, since partner attitudes will likely influence its use in women,”
she says.
Because this is a Phase 1 study, the
clinic will recruit mostly healthy volunteers but also plans to
include a small number of HIV-positive women to determine whether
use of the gel will reduce viral loads in the vaginal tract, which
might mean the agent could reduce the potential for infected people
to spread the virus to uninfected contacts.
The CDC is contracting with other
sites to study microbicides in men, but they have asked the Hope
Clinic to focus on women volunteers for its studies, says Priddy.
“Until we have a vaccine that
we can administer to everyone, it would be better if we could give
people, particularly women, an option
besides condoms,” she adds. “In many other countries,
and in some populations in the United States, women don’t
feel able to ask their partner to use a condom. A microbicide could
put protection entirely in their hands. They could decide to use
protection, and their partner might not necessarily have to know
about it.” option
besides condoms,” she adds. “In many other countries,
and in some populations in the United States, women don’t
feel able to ask their partner to use a condom. A microbicide could
put protection entirely in their hands. They could decide to use
protection, and their partner might not necessarily have to know
about it.”
This is not the first time
that scientists have attempted to use topical agents to combat HIV,
she notes. For years, clinicians knew that the spermicide nonoxynol-9
had antiviral properties, and labstudies showed that it was effective
in inactivating HIV.
However, clinical studies among commercial
sex workers—who used the agent several times a day—showed
that users actually contracted HIV at higher rates than non-users.
Nonoxynol-9 used that frequently caused skin breakdown that made
the women more vulnerable to infection, not less.
“That is why these trials in
healthy volunteers at low risk are so important,” Priddy emphasizes.
“We don’t want to promote something that will actually
have the result of leaving them more susceptible than they were
before."
|
|
 |
| |
|
|
|
|
| |
Computer
screening saves lives
Patients
seeking care
in the emergency room at Grady Memorial Hospital are also being
screened for signs of depression, domestic violence, and post-traumatic
stress disorder (PTSD) under an innovative research program conducted
by a member of Emory’s
care
in the emergency room at Grady Memorial Hospital are also being
screened for signs of depression, domestic violence, and post-traumatic
stress disorder (PTSD) under an innovative research program conducted
by a member of Emory’s
emergency medicine faculty.
Debra Houry, an
assistant professor of emergency medicine, is conducting research
on the incidence of PTSD and depression among victims and perpetrators
of domestic violence by
using an interactive computer kiosk stationed in the hospital’s
emergency department (ED).
Participants in the study receive
needed referrals and information if their computer evaluation shows
they are at risk for domestic violence, suicide, or PTSD.
Two days a week, all ED patients between
the ages of 18 and 55 are approached by a research assistant and
asked if they want to participate in a voluntary study by answering
a computerized questionnaire at the kiosk.
Based on their answers, Houry and
her colleagues are able to offer information about services that
can help, arrange for confidential follow-up visits, or—in
the case of patients whose evaluation indicates suicidal ideation
or intent—arrange immediate treatment.
Too often, people in abusive situations
are too ashamed or
fearful to openly seek help, Houry says. One of the good things
about the kiosk project is that it can screen people who are in
the ED seeking care for another problem and offer them
immediate assistance.
“In terms of domestic violence,
many patients did not realize they were victims until we told them
that being beaten is not normal relationship behavior,” she
says. “A lot of them now are taking more ownership and feel
more empowered, and that is something I am very pleased with.”
Signs of abuse, depression, and anxiety
disorders might not be evident to a busy emergency physician, especially
if the patient is seeking treatment for an unrelated problem. The
kiosk program makes use of the downtime the patient or family member
must spend in the waiting room to collect additional information.
With the person’s consent, the
information collected by the computer program can then be shared
with his or her treating physician.
Houry’s research using the kiosk
program is part of a $1.6 million study funded by a three-year grant
from the Centers for Disease Control and Prevention and a five-year
grant from the National Institute of Mental Health. The CDC portion
of the grant is for research to find safe ways to screen for domestic
violence and to follow up with reported victims, and the NIMH portion
is dedicated to studying the possible relationship between mental
illness and domestic violence.
With just over a year’s worth
of data collected, Houry says she has noticed a significant correlation
between domestic violence and suicidality, PTSD, and symptoms of
depression.
Of the patients enrolled in the study
so far, 38% were victims of domestic violence, with 39% of men reporting
themselves as victims. Twenty-nine percent of men in the study reported
being perpetrators. Of all patients, 27% experienced moderate to
severe depression, 15% reported having moderate to severe PTSD symptoms,
and 7.5% were suicidal.
“In general, we have observed
significant amounts of depression and post-traumatic stress disorder
among our patients here at Grady. I think a lot of that has to do
with the ongoing challenges they have on a daily basis, with poverty
and being surrounded by violence much of the time,” Houry
says. “But the incidence of depression and suicidality have
been much higher in both victims and perpetrators of domestic violence
when compared with the rest of our patient population.”
Since the beginning of the kiosk program,
Houry notes that several female patients have left violent relationships,
more than 50% have developed safety plans, and almost all have kept
and used the resource lists they received when they were screened.
“With just our preliminary data,
we are finding that we are making a big difference in people’s
lives.”
|
|
 |
| |
|
|
|
| |
| |
|
|
|
|
|
|
| |
Milestones
Emory University
researchers
attracted $351.5 million in external research funding in fiscal
year 2004, leading Georgia’s research institutions in funding,
and increasing research awards by approximately 10% over fiscal
year 2003. Emory’s Woodruff Health Sciences Center (WHSC)
received more than 93% of the total, at $328.9 million. Federal
funding was responsible for 71.3% of WHSC funding, with fund-ing
from the NIH making up 62.5% of the WHSC total and 87.7% of its
federal funding.
|
|
| |
| |
|
|
| |
THE
ROLLINS SCHOOL
OF PUBLIC HEALTH
has been awarded a total of $6.3 million in grants from the
Centers for Disease Control and Prevention to establish programs
at a new Cancer Prevention Research Center. Three-quarters
of a million Georgians are expected to benefit from this major
new public health initiative aimed at reducing high cancer
rates through education programs that target smoking, obesity,
and lack of physical fitness. The center will focus its efforts
on improving the health of residents in the 33 counties of
southwest Georgia. The core grant of $3.8 million supports
a partnership of the Woodruff Health Sciences Center and the
Southwest Georgia Cancer Coalition. In addition, a five-year
grant of $1.6 million will aid Emory’s effort to be
part of a Cancer Prevention and Control Research Network,
and a three-year grant of $900,000 will be used to improve
quality of life for men with localized prostate cancer.
|
|
 |
|
|
| |
|
|
|
|
| |
Gastrointestinal
surgeons
at Emory Crawford Long Hospital and Emory University Hospital are
among the first in the world to treat patients suffering from gastroesophageal
reflux disease (GERD) with a simple, outpatient endoscopic procedure
that takes less than an hour. Undergoing the new procedure does
not complicate future surgery for patients who do not experience
relief but provides another treatment option for patients who would
not do well with traditional surgery or those who want an intermediate
option between medication and surgery.
New
treatments for devastating illnesses such as cancer, HIV,
Alzheimer’s, and cardiovascular disease could reach patients
sooner thanks to the new Venture Lab program in Emory University’s
Office of Technology Transfer. Venture Lab will identify potentially
marketable Emory Research discoveries in their early stages and
help find the funding necessary to bring the technologies to market.
The President’s Emergency
Plan for AIDS Relief (PEPFAR) has given a $12 million grant to
transfusion
medicine experts
at Emory
University, the American Association of Blood Banks, and the American
Red Cross to improve the safety of blood transfusion in the African
countries of Kenya, South Africa, Mozambique, and Ghana. The goal
is to significantly decrease the incidence of HIV transmitted through
transfusion and to ameliorate the devastating personal, social,
economic, and political effects of HIV in those nations.
Relief (PEPFAR) has given a $12 million grant to
transfusion
medicine experts
at Emory
University, the American Association of Blood Banks, and the American
Red Cross to improve the safety of blood transfusion in the African
countries of Kenya, South Africa, Mozambique, and Ghana. The goal
is to significantly decrease the incidence of HIV transmitted through
transfusion and to ameliorate the devastating personal, social,
economic, and political effects of HIV in those nations.
Emory
University Hospital (EUH) has been recognized as a National
Research Corporation (NRC) Consumer Choice Award winner for the
seventh year in a row. EUH is the only hospital in Atlanta and one
of only two in Georgia to be honored this year. Consumer Choice
Awards recognize those hospitals that are named by health care consumers
as having the highest quality and image in 154 markets throughout
the country.
|
|
| |
|
|
|
|
| |
| |
|
|
| |
EMORY
HEALTHCARE'S
information technology department has been recognized for
an innovative project that connects hundreds of computer servers
and thousands of desktops into one large virtual pool of memory.
A report detailing the design has been accepted into the global
Archives of the Computerworld Honors Collection.
Computerworld is a weekly magazine described as “the
voice of IT management” for Fortune 1000 companies.
|
|
 |
|
|
 |
| |
|
|
|
| |
| |
Targeting
hard-to-treat tumors
Patients receiving radiation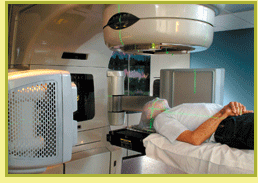
therapy at Emory’s Winship Cancer Institute are the
first in the nation treated with new technology that allows doctors
to use real-time images to directly target certain tumors while
leaving nearby healthy tissue untouched.
Last June, the medical school’s
Department of Radiation Oncology became the first department in
the United States to use the new On-Board Imager (OBI), developed
by Varian Medical Systems, to treat patients with brain tumors as
well as head, neck, and prostate cancer. Emory is also the first
center in the world to combine use of the OBI and Varian’s
new medical linear accelerator to perform new procedures in stereotactic
radiosurgery.
The OBI allows medical personnel to
visualize tumors at the time of treatment, repositioning patients
on the table, if necessary, to precisely direct the radiation beam.
Use of the imager represents the “next
wave of treatment delivery options in this field,” says Timothy
Fox, the department’s chief medical physicist.
State-of-the-art, image-guided radiation
therapy (IGRT) uses techniques like three-dimensional CT scans and
intensity-modulated radiation therapy (IMRT) to target tumors once
thought untreatable.
The 3-D scans provide high-quality images of the tumors and surrounding
normal tissue, and IMRT allows oncologists to create treatment plans
that vary the intensity of radiation to match the exact shape of
tumors and avoid high doses to other critical areas of the body.
Without OBI, however, treatment plans
are often executed based on information obtained in CT scans taken
days before treatment,  though
specialists know that some tumors often change position on a daily
basis, Fox says. though
specialists know that some tumors often change position on a daily
basis, Fox says.
Traditionally, clinicians must also
rely on external skin marks with laser systems to guide patient
positioning the actual day of treatment. Patient placement is determined
by aligning the treatment beam with the external marks and comparing
with the older CT scan.
Using the OBI, two x-ray images are
taken of the patient’s treatment area shortly before radiation
is initiated. Aided by a computer, these images are either manually
or automatically matched with the reference images from treatment
planning. The system then calculates how much the treatment table
should move to align the tumor with the beam. The treatment couch
can then be adjusted to accommodate any changes in tumor position.
“This technology allows us to
be more precise with our treatment delivery,” Fox says. “It
allows us to see the tumors and better target them while avoiding
the nearby critical structures.”
The imager will also allow better
treatment of tumors that move, such as those in the lung or liver,
which change position as the patient breathes.
In current practice, radiation is
delivered to encompass the tumor’s movement, meaning that
healthy tissue is also irradiated. But using the OBI combined with
an Emory-pioneered technique called “gating,” oncologists
will be able to time delivery of the radiation to just those moments
that the tumor is in line with the beam.
Used in conjunction with a new medical
linear accelerator, known as Trilogy, the imager is also allowing
Emory doctors to pioneer new techniques in stereotacticradiosurgery,
an ultra-precise form of radiation therapy that allows improved
targeting and high-dose treatment of brain tumors.In October, Emory
radiation oncologist Ian Crocker used the machine to treat two small
cancer metastases in the brain of a 56-year-old breast cancer survivor.
The single procedure delivered a radiation beam so powerful andtightly
focused that it is considered radiosurgery instead of radiation
therapy, Crocker says.
“Given her favorable long-term
outlook, we were committed to delivering a focal, high-dose radiation
treatment to eliminate the risk of brain injury from radiation treatment
to the whole brain,” Crocker says.
Had the woman been treated a month
earlier, she would have received the standard treatment of low-dose
radiation therapy to her entire brain, a procedure that would have
less chance of effectively treating the tumors and a higher risk
of complications.
As department chairman Lawrence Davis
notes: “Using the Trilogy system, we have the potential to
substantially improve cancer treatment outcomes by doing a better
job of protecting healthy tissue while delivering more powerful
doses to the tumor.”
|
|
 |
| |
|
|
|
| |
| |
|
|
|





 will lead to a
safer health care environment, administrators say.
will lead to a
safer health care environment, administrators say. 2 billion people worldwide lack access to safe drinking water, and
more than 1 million people die each year of water-transmitted diseases.
2 billion people worldwide lack access to safe drinking water, and
more than 1 million people die each year of water-transmitted diseases.
 Gangarosa
began his public health career in 1959 as one of the first doctors
working on the international fight against cholera. At the time,
data from the World Health Organization indicated that waterborne
diseases annually killed almost 5 million people.
Gangarosa
began his public health career in 1959 as one of the first doctors
working on the international fight against cholera. At the time,
data from the World Health Organization indicated that waterborne
diseases annually killed almost 5 million people. healthy 40-year-olds have immune systems that look like that of
an 80-year-old? And how does this influence their risk of developing
cancer, heart disease, or Alzheimer’s later in life?
healthy 40-year-olds have immune systems that look like that of
an 80-year-old? And how does this influence their risk of developing
cancer, heart disease, or Alzheimer’s later in life?

 Pediatrics and medical director of Children’s Healthcare of
Atlanta at Egleston.
Pediatrics and medical director of Children’s Healthcare of
Atlanta at Egleston. positions
as head of computed tomography and vice chair of radiology for health
systems
positions
as head of computed tomography and vice chair of radiology for health
systems 
 option
besides condoms,” she adds. “In many other countries,
and in some populations in the United States, women don’t
feel able to ask their partner to use a condom. A microbicide could
put protection entirely in their hands. They could decide to use
protection, and their partner might not necessarily have to know
about it.”
option
besides condoms,” she adds. “In many other countries,
and in some populations in the United States, women don’t
feel able to ask their partner to use a condom. A microbicide could
put protection entirely in their hands. They could decide to use
protection, and their partner might not necessarily have to know
about it.” care
in the emergency room at Grady Memorial Hospital are also being
screened for signs of depression, domestic violence, and post-traumatic
stress disorder (PTSD) under an innovative research program conducted
by a member of Emory’s
care
in the emergency room at Grady Memorial Hospital are also being
screened for signs of depression, domestic violence, and post-traumatic
stress disorder (PTSD) under an innovative research program conducted
by a member of Emory’s 
 Relief (PEPFAR) has given a $12 million grant to
transfusion
medicine experts
at Emory
University, the American Association of Blood Banks, and the American
Red Cross to improve the safety of blood transfusion in the African
countries of Kenya, South Africa, Mozambique, and Ghana. The goal
is to significantly decrease the incidence of HIV transmitted through
transfusion and to ameliorate the devastating personal, social,
economic, and political effects of HIV in those nations.
Relief (PEPFAR) has given a $12 million grant to
transfusion
medicine experts
at Emory
University, the American Association of Blood Banks, and the American
Red Cross to improve the safety of blood transfusion in the African
countries of Kenya, South Africa, Mozambique, and Ghana. The goal
is to significantly decrease the incidence of HIV transmitted through
transfusion and to ameliorate the devastating personal, social,
economic, and political effects of HIV in those nations.
 though
specialists know that some tumors often change position on a daily
basis, Fox says.
though
specialists know that some tumors often change position on a daily
basis, Fox says.