2003 Georgia General Assembly
Nonphysician visits on the rise
Milestones
Neurointensive care saves
Human, $ toll of HIV rising
Bad rap


National security
Open records/security exceptions
SB 113 amends the open record/ meeting statute to exempt from disclosure
those records or meetings that would compromise security against sabotage
or criminal or terrorist acts. Specific exemptions include plans for
bioterrorism response and the national pharmacy stockpile.

Tobacco taxes up
Cigarette taxes rose by 25 cents per pack (from 12 cents to 37 cents). Taxes on cigars were upped 13% to 23%, and a new 10% tax on smokeless tobacco was approved. Together, the new tobacco taxes resulted in an additional $180 million in new monies for the state.



The
good news
The House and Senate recognized Emory Hospitals for leadership and innovation
in patient safety.
The bad news
Physicians and hospitals will receive reduced Medicaid and Peachcare
reimbursements in 2004.
Looking ahead
Emory will continue to advocate for medical malpractice liability reform
in the 2004 General Assembly.


Civil justice?

Class action legislation inched Georgia forward (although only slightly)
toward civil justice reform. HB 792 included language designed to prevent
frivolous lawsuits by limiting the number of times to one that a plaintiff
can dismiss a case and by prohibiting all dismissals after jury selection.
Also, the interest rate on judgments was reduced from the 12% fixed
rate to prime plus 3%.


By Linda Womack
 While the 2003 Georgia General Assembly proved historic on many
fronts - the first Republican governor in 130 years, a new speaker of
the House, and a Republican majority in the Senate - the longest legislative
session in 100 years will probably be best remembered at Emory for painful
cuts, particularly in the Medicaid program. A last-minute tobacco tax
increase made up for some budget shortfalls. Unresolved were issues
such as civil justice reform (in layman's terms known as tort reform
or medical liability reform) which, if passed, would have addressed
continuing increases in medical liability premiums.
While the 2003 Georgia General Assembly proved historic on many
fronts - the first Republican governor in 130 years, a new speaker of
the House, and a Republican majority in the Senate - the longest legislative
session in 100 years will probably be best remembered at Emory for painful
cuts, particularly in the Medicaid program. A last-minute tobacco tax
increase made up for some budget shortfalls. Unresolved were issues
such as civil justice reform (in layman's terms known as tort reform
or medical liability reform) which, if passed, would have addressed
continuing increases in medical liability premiums.
Money matters
Because of the continued decline in state revenues over the past 18 months, legislators were faced with a projected $750 million shortfall in the FY 2004 budget. To balance the budget as required by Georgia law, legislators cut millions. On the final day of the session, lawmakers agreed to an omnibus tax bill that included a version of the governor's proposed tobacco tax, which added $180 million in new monies, along with another $400 million through other measures. The additional revenue prevented even more cuts in the budget, but no new programs were created, and there were few enhancements to existing programs.
Along with other health care organizations and advocates, the Woodruff Health Sciences Center, Emory Healthcare, Emory School of Medicine, Rollins School of Public Health, and the Nell Hodgson Woodruff School of Nursing supported the governor's legislation and joined the Tobacco Tax Coalition, which backed a proposed 75 cents per pack increase in cigarette taxes.
The state's 2004 budget totaling $16 billion was effective July 1 and is particularly important to Emory physicians and hospitals, which now must now live with 10% less in Medicaid or Peachcare reimbursements while continuing to provide health care to low-income adults and children. For hospitals, that cut originally translated into a $75 million net cut statewide (or closer to home, $1.14 million less in reimbursements for Emory Hospitals). The hospital cut was partially restored by some shifting of tobacco settlement money from the Department of Education's school nurse program to the Department of Community Health. DCH will use these Medicaid dollars (approximately $30 million) and match with federal dollars, and hospitals will then repay the school nurse program through state health benefit plan contracts. Georgia physicians who are Medicaid providers would net $45.3 million less from both state and federal funds, including about $1 million less for Emory physicians.
Monthly payments to physicians participating in the Georgia Better Health care program (a primary care case management program directly administered by the DCH to improve access to medical care) were reduced from $3 per member per month to $2 for a total of $8 million in cuts. Primary care providers have been receiving a $3 per member per month case management fee for coordinating members' health care services. When services are provided, the regular fee for reimbursement applies. The budget includes funds for an inflationary increase for hospital inpatient rates at 3.2% and 4.5% for physician and physician-related services.
Other budget items of interest to the Woodruff Health Sciences Center included maintaining funding for the Georgia Cancer Coalition at the FY 2003 level of almost $31 million. The Georgia Research Alliance received funding at more than $23 million. Additionally, the Emory School of Medicine will continue to receive funding through these Georgia Board for Physician Workforce programs, although at slightly reduced levels for the most part:
- Medical student capitation - $993,157 for 113 Georgia students @ $8,789 per slot.
- Family practice residency capitation - $473,760 for 24 residents @ $19,740 per slot.
- Student preceptorships - $15,000 for 10 @ $1,500 per slot.
- Preventive medicine - $18,800 for two students @ $9400 per slot. The Rollins School of Public Health will receive funding at the same level for four residents.
Still no reform
While the budget is always at the top of the list on the Woodruff Health Sciences Center's state legislative agenda, the priority issue for the 2003 Georgia General Assembly was civil justice reform. With Emory Healthcare shouldering annual double-digit increases in medical liability premiums - 17% in fiscal year 2002, another 48% in 2003, and now a projected increase of 45% in 2004 - this will continue to be our number one legislative issue for the 2004 session. In coordination with the Georgia Chamber of Commerce, the Medical Association of Georgia, and the Georgia Hospital Association, our lobbying efforts supported the provisions of SB 133, which would have meaningfully addressed the continued increases and high cost of medical malpractice insurance. SB 133 was watered down considerably in the Senate, and a hearing was never called by the House judiciary committee chairman.
As we are unable to raise charges to defray the rising costs of medical liability insurance because of the constraints on Medicare, Medicaid, and managed care reimbursements, the ability of Emory Healthcare and other health care providers throughout the state to serve Georgia's 8 million citizens is threatened. As introduced, SB 133 would have balanced a patient's access to the courts with access to quality health care.
We will continue our efforts for passage of meaningful civil justice reform legislation in 2004, including these provisions:
- $250,000 cap on noneconomic damages (pain and suffering)
- An expert witness must be actively teaching in the same field or specialty as the defendant for at least three of the five years before the alleged negligence occurred. This would apply not only to medical practitioners, but to all licensed professionals within the state, such as architects, engineers, and attorneys.
- An emergency room provision would ensure that hospitals or health care providers who treat a patient during the first 24 hours of an emergency medical condition or an unscheduled hospital visit would not be liable for noneconomic damages resulting from an act or omission in delivering that care or treatment. Hospitals do not have ready access to patients' medical records or histories in the emergency room. This protection would not apply in cases of willful or wanton misconduct or gross negligence.
- Eliminate joint and several liability so that the defendant is responsible only for his or her degree of fault.
- Establish comparative negligence so that defendants cannot be held liable if the plaintiff is 50% or more responsible for the injury; also require that awards be reduced by the percentage the plaintiff is found at fault.
Without these important provisions, doctors, hospitals, and nursing homes throughout Georgia will continue to face the challenge of providing quality patient care while bearing the financial burden of skyrocketing insurance premiums due to more claims and ever-rising jury awards.
In addition to my daily contact regarding this issue with legislators, individual interactions that many of our trustees, members of the Emory Healthcare Board, physicians, and other Emory colleagues had with their respective legislators were helpful and appreciated. These efforts are so important, and I look forward to working with our Emory Healthcare community in a grassroots campaign as we move this issue forward in 2004.
Other measures that affect us
Many other important health care-related measures passed and were signed into law:
- Nursing home provider tax. A fee on all nursing home providers in the state will be used to obtain additional federal matching revenue. With these funds, the 10% reimbursement rate reductions for Medicaid nursing homes will be restored in the state's FY 2004 budget. Most important to Emory Healthcare's two Wesley Woods facilities (Budd Terrace and Wesley Woods Newnan in Peachtree City) is the provision requiring the Department of Community Health to submit a waiver of uniformity to the US Department of Health and Human Services. Unless waived as permitted by federal law, the uniformity requirement would require facilities like Wesley Woods, which do not receive any Medicaid funds, to pay the tax at the same rate as Medicaid providers that will benefit from Medicaid funds raised by the tax.
- Bioterrorism and animal diseases. SB 183 makes it a misdemeanor of a high and aggravated nature for any person to knowingly introduce any foreign animal disease or any animal disease, syndrome, chemical, poison, or toxin that may pose a substantial threat or harm to the animal industries in Georgia. The federal government, through the US Patriot Act and the Public Health Security and Bioterrorism Preparedness and Response Act, regulates Emory's research of many agents on the list. SB 183 allows bona fide research by or on behalf of any public or private college or university in Georgia and exempts them from the reporting requirements.
- Veterinarian Practice Act. This exempts private and public research universities from the provisions of the rewritten Veterinarian Practice Act.
- Dangerous drug update/controlled substances. HB 261 provides that a prescription for a dangerous drug is not required to bear the Drug Enforcement Administration permit number of the prescribing practitioner. However, it must include the name and strength of the drug, the quantity to be dispensed, and the printed name, address, telephone number, and signature of the practitioner.
- Off-label prescription drug coverage. SB 96 requires insurance companies to cover off-label prescription drugs used for a purpose or indication not approved by FDA.
- Vaccination program for emergency responders. SB 333 (attached to HB 372) requires the Department of Human Resources (DHR) to offer a vaccination program to emergency responders when funds are available for the program. Emergency personnel would be vaccinated only if their jobs expose them to blood-borne pathogens. Personnel can elect not to be vaccinated for personal or religious reasons. DHR rules and regulations supersede county health regulations.
- Smallpox immunity. SB 336 (attached to HB 372) provides legal immunity to hospitals and health care workers through their participation in smallpox vaccination and treatment programs, however, only in the absence of gross negligence or willful or wanton misconduct.
- Social Security number on insurance cards. HB 721 prohibits insurers from displaying the insured's social security number on insurance identification cards.
For additional information about these and other measures affecting Emory, please contact Linda Womack at lwomac2@emory.edu or 404-727-5306. Or see http://www.legis.state.ga.us/.
Linda Womack is director of state affairs in Emory's Office of Governmental
and Community Affairs.
More News and Milestones

Patients are increasingly being treated by multiple providers who have a wide range of training and philosophical approaches.
Nonphysician visits on the rise
Between 1987 and 1997, the proportion of patients in the United States
who visited nurses, chiropractors, podiatrists, optometrists, and other
nonphysician clinicians rose from 30% to 36%, says Benjamin Druss, Rosalynn
Carter Chair of Mental Health at the Rollins School of Public Health.
 Patients are increasingly treated by multiple providers who have
a range of training and philosophical approaches, Druss and his co-authors
note in a recent issue of the New England Journal of Medicine.
Patients are increasingly treated by multiple providers who have
a range of training and philosophical approaches, Druss and his co-authors
note in a recent issue of the New England Journal of Medicine.
During a ten-year study that drew on more than 40,000 patient interviews, nonphysicians were more likely to provide preventive services, less likely to diagnose and treat specific illnesses, and more likely to work in the same location as a physician. This suggests that nonphysicians and physicians are working together to care for patients. There were also more nonphysician clinicians graduating from training programs, more state laws allowing nonphysicians a greater scope of clinical practice, and more managed care plans that used these providers to control costs. "Multidisciplinary teams can improve care," says Druss, "particularly for chronic conditions, but only if that care is carefully coordinated. Without effective communication, provision of care by multiple providers can reduce continuity and quality of care."

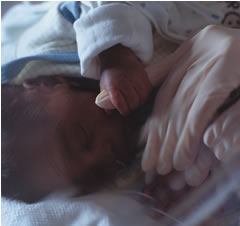
What's best in Atlanta? When a series of 30 second commercial spots on the CBS affiliate Channel 46 posed that question, Emory Crawford Long Hospital's answer was its level 3 neonatal intensive care unit (NICU). Premies in the NICU - some weighing less than two pounds - receive the highest level of developmental care, in conditions closely emulating those in the womb.
Some 2,400 babies a year are delivered in ECLH's new Women's Center, where there are private suites for all mothers and facilities to accommodate 16 premature babies. As the television spots observed, "It's not just the best place for mothers, it's the best place for babies."

Milestones
A one-capsule-a-day medication discovered at Emory for the treatment of HIV was approved by the Food and Drug Administration for commercial use. Emtriva (emtricitabine), to be marketed and distributed by Gilead Sciences, was invented by Emory scientists Raymond Schinazi (pediatrics), Dennis Liotta (chemistry), and Woo-Baeg Choi (president of FOB Synthesis, a drug discovery company at EmTech Bio on Emory's Briarcliff campus).
Thanks to cardiologist Christopher Cates of the Emory Heart Center at Hiawassee, a resident of Blairsville was the first in north Georgia to benefit from a new breakthrough in heart disease treatment, the recent FDA approved drug-eluting CYPHER stent.
Two Emory obstetricians/gynecologists at Grady Hospital - Kimberly Kleiss and Michael McCall - are among the first in the country to use microculdoscopy to help diagnose ectopic pregnancies.
Researchers in the School of Medicine led the nation in April in demonstrating the validity of a rapid laboratory test to diagnose SARS (Severe Acute Respiratory Syndrome). The polymerase chain reaction test in pathologist Frederick Nolte's molecular diagnostic lab took about four hours to confirm the presence of the SARS virus in a sample from a German lab.
Corneal specialist Doyle Stulting performed the first artificial corneal transplant in the United States in May. The Emory Eye Center and the Cincinnati Eye Institute are the first sites to use the new synthetic keratoprosthesis (artificial corneal device) developed by Argus Biomedical in Australia.
U.S. News & World Report named Emory University Hospital one of America's best hospitals in seven specialties. Named in the top 50 are heart and heart surgery (7), eyes (15), psychiatry (17), kidney disease (28), urology (32), gynecology (39), and geriatrics (41). Each of those programs were the only ones in Georgia listed in their specialty areas.



Neurointensive care saves
Stroke patients have had shorter hospital stays and better clinical outcomes since Emory University Hospital's neurointensive critical care unit - the only one in the state - was established in 1998.
The mean length of stay for neurological and neurosurgical patients admitted to the unit between April and September 1998, 1999, and 2000 dropped by 30% to 34%, according to a recent study. Since the unit was established, the mean number of patient-ventilator days also has dropped -- from 17 days in 1997-1998 to 11 days. Ventilator-associated mortality fell 76%. Researchers also looked at severity-adjusted data, comparing expected length of stay to observed length of stay. The University Hospital Consortium considers this severity-adjusted data a benchmark of quality of care.
During the review, the NICU staff included fellowship-trained neurointensive care physician Owen Samuels, two nurse practitioners, a pharmacist, respiratory therapist, nutritionist, and postgraduate neurology and neurosurgery residents. A second neurointensivist Mustapha Ezzeddine recently joined the team, as demand for this specialty in critical care continues to increase.
"The results of the Emory study are consistent with data that show that intensive care specialists can help reduce mortality, improve clinical outcomes, and save hospitals millions of dollars while saving the lives of critical care patients," says Samuels, who led the study. "But this type of care is not the standard across the United States."
The findings of the study are consistent with the larger, more established practice of using intensivists in general medical and surgical ICUs, says Samuels.

Human, $ toll of HIV rising
Failure to reduce new HIV infections in the United States by 50% in the next two years will have substantial human consequences and could cost this nation more than $18 billion, says health economist David Holtgrave of the Rollins School of Public Health. Failure to meet the Center for Disease Control and Prevention's national goal of reducing new HIV infections by 50% by 2005 would result in 130,000 additional HIV infections between now and 2010.
The CDC needs $300 million to $334 million in additional resources for the next four fiscal years, says Holtgrave, to expand HIV counseling and testing, behavioral risk reduction services for persons at risk of HIV infection through sexual contact or substance abuse, and intensive prevention services for persons already living with HIV.



In this issue
From the CEO / LettersPromises writ in stone
Taking care of people
Taming the obNOXious enzyme
Moving forward
Noteworthy
On Point:
Communicating medical errors

Bad rap
Risky behavior and a heightened incidence of sexually transmitted diseases among African-American female adolescents may be linked to high exposure to rap music videos, according to a study in the March issue of the American Journal of Public Health. Despite concern about the themes and images expressed in rap music videos, there's been limited research on their impact on adolescents' behavior. Gangsta rap in particular, the researchers say, "is explicit about sex and violence, but rarely shows the potential long-term adverse impact of these risky behaviors."
In their study of 522 unmarried African-American female adolescents, ages 14 to 18, who lived in nonurban, lower socioeconomic neighborhoods, sociologist Gina Wingood of the Rollins School of Public Health and her colleagues at Emory and the University of Alabama at Birmingham found that adolescents exposed to 14 or more hours per week of rap music were three times more likely to hit a teacher and more than 2.5 times as likely to have been arrested, compared with their peers with less exposure to rap. Adolescents who frequently watched rap videos during the 12-month study were twice as likely to have multiple sexual partners, and more than 1.5 times as likely to acquire a sexually transmitted disease and use drugs and alcohol.
"Adolescents want to be autonomous and independent from parental controls, an act that can be viewed as somewhat defiant," says Wingood. "They may also be modeling what they see as the norm. They pattern themselves after their peers and the women they consider to be role models on the videos. On the other hand, it may be an attempt to defy the white mainstream popular culture, since rap music is more ethnocentric."
Copyright © Emory University, 2003. All Rights Reserved.
Send comments to the Editors.
Web version by Jaime Henriquez.