













|
 |
 |
|
|
|
A
Legacy of Firsts
Bellamy
receives Emory Medal
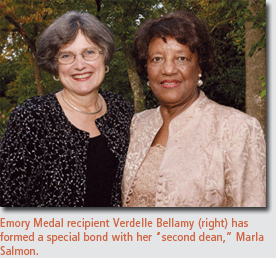
 hose who know Verdelle Bellamy, 63MN, no doubt regard her as a quiet
but determined pioneer whose influence continues to have far-reaching
effects in the field of nursing. Bellamy, the first African American
to graduate from Emory, was honored last fall with an Emory Medal,
the university’s highest honor for alumni.
hose who know Verdelle Bellamy, 63MN, no doubt regard her as a quiet
but determined pioneer whose influence continues to have far-reaching
effects in the field of nursing. Bellamy, the first African American
to graduate from Emory, was honored last fall with an Emory Medal,
the university’s highest honor for alumni.
“I’m
so proud to be your twin tonight,” said Charles Haynes, 71C,
85PhD, a preeminent First Amendment scholar who received an Emory
Medal along with Bellamy.
As Bellamy accepted the honor, she
used the occasion to reflect on the past. “I stand on the
shoulders of Emory, and I’m also standing on the shoulders
of Ada Fort, a pioneer firm in her convictions and beliefs.”
Bellamy was referring to the nursing school dean who, together with
Henry Bowden, chair of the university’s Board of Trustees,
led the fight to admit African American students to Emory. It was
Bowden who took the battle to the courts to change the law prohibiting
private schools like Emory from admitting black students.
Bellamy also paid homage to her mother
and grandmother for imbuing her with self-confidence and strong
Christian values. Bellamy developed a sense of quiet determination
at a young age. She admired the public health nurse at her elementary
school in Alabama and aspired to become a nurse herself, though
her family wanted her to become a teacher. She graduated from Tuskegee
Institute (now university) in 1958 and went on to receive a diploma
degree in nursing from Grady Memorial Hospital. She was teaching
there in 1962 when Fort somehow found her and Allie Saxon, a friend
of Bellamy’s who brought high school vocational nursing students
to Grady for clinical experience. Thanks to the efforts of Fort
and other supporters, Bellamy and Saxon enrolled in the nursing
school in 1963, thus becoming the first black students to study
full time at Emory.
After Bellamy graduated from Emory,
her skin color made it difficult for her to find a job at the Veterans
Affairs Medical Center (VAMC) in Atlanta, where she was told no
positions were available, despite vacancies within the VA and her
previous experience at the VA center in Tuskegee. Bellamy persisted
and was eventually hired as coordinator of medical services and
surgical services at the Atlanta VAMC. She rose to the rank of associate
chief of nursing services, the first black employee to be appointed
to an administrative position at the Atlanta center. She designed
and implemented policies and procedures for the 120-bed long-term
care unit that ultimately became a model for VA centers around the
country. Other firsts for her included being the first black elected
to the executive committee of the Georgia Nurses Association (1971),
receiving a gubernatorial appointment to the Georgia Board of Nursing
(1974), and being elected president of the Georgia Board of Nursing
(1978).
Bellamy also served as national president
of Chi Eta Phi Sorority, a professional association for registered
professional nurses and students, from 1973 to 1977 and was inducted
as a fellow in the American Academy of Nursing in 1993.
In 2001, she worked with School of
Nursing Dean Marla Salmon to diversify the school’s student
population. By 2004, one-third of the incoming class represented
minority groups.
Bellamy’s husband, Monroe, and
her son, Michael, were with her the night she received the Emory
Medal, as was Salmon, whom Bellamy described as “my second
dean.”
“My life has been blessed because
of you,” Bellamy said from the podium. “How do I say
thank you? There’s nothing I cherish more than the Emory Medal.”
|
 |
| |
|
|
|
| |
|
|
|
 |
|
| |
More Research Momentum

 r. Kenneth Hepburn recently joined the School of Nursing
as associate dean for research. He held a similar position
with the School of Nursing at the University of Minnesota,
where his studies included caregivers for family members
with dementia, geriatric team care, education and evaluation
issues, and change of practice behavior.
r. Kenneth Hepburn recently joined the School of Nursing
as associate dean for research. He held a similar position
with the School of Nursing at the University of Minnesota,
where his studies included caregivers for family members
with dementia, geriatric team care, education and evaluation
issues, and change of practice behavior.
“I came to Emory because it seemed an extraordinary
opportunity to help a strong program advance its agenda
of nursing science,” says Hepburn. The main task ahead:
helping achieve the goals set forth in the faculty-authored
plan “Becoming the Best in Research.”
“This means working with faculty and the school’s
leadership to recruit more researchers to our faculty, strengthening
support systems for faculty to conduct their research, and
providing mentoring, especially to junior faculty,”
says Hepburn, who is meeting his counterparts at Emory and
other universities to strengthen research collaborations.
He also serves as educational core director of the Emory
Alzheimer’s Disease Center.
|
|
| |
|
|
|
|
| |
|
|
|
| |
|
|
|
| |
|
A
New Century of Possibilities
Nursing
school caps its centennial year

 an
you imagine a world without nurses?” an
you imagine a world without nurses?”
The question, posed by Woodruff Health Sciences Center CEO Dr. Michael
Johns in a video about the School of Nursing, made for the perfect
segue as Dean Marla Salmon addressed more than 200 guests attending
the capstone event of the school’s Centennial Celebration.
“Unfortunately, it’s no
longer unimaginable to need care and not have a nurse available
as our country and the world face the worst nursing shortage ever,”
said Salmon.
“We are the lucky ones,” she
added, referring to the growing number of baby boomers who are retiring
from nursing. “In many of the world’s poorer countries,
large numbers of nurses are dying of infectious disease or are walking
away, exhausted by what is asked of them. Many of these nurses come
to fill the gaps here in our country. Who will be there to care
for the patients that they leave behind?”
Everyone in the room—students,
faculty, staff, alumni, Emory administrators and trustees, and supporters
from the corporate and Atlanta communities—knew the answer.
All had come to pay homage to the past and look ahead to the future
as the School of Nursing embarks on its second century.
There was much to reflect upon. The
school’s founding as the Wesley Memorial Hospital Training
School for Nurses in 1905. The development of its undergraduate,
master’s, and doctoral programs. Its commitment to gender,
racial, and ethnic diversity. Strong collaborative partnerships
to improve health and health care locally, nationally, and globally.
Consistent rankings that place Emory among the top 10% of nursing
schools nationally. And more.
But what really matters, Salmon pointed
out, “is that we live out our potential to truly improve nursing’s
ability to care. We do aspire to be great, but we never forget that
our real job is to do good.”
The potential for good rests in the
hands of Emory’s future nurses, whose numbers—400 undergraduate
and graduate students—have nearly doubled since 1999.
Nursing senior Donté Flanagan,
who is intent on becoming a pediatric nurse, is among them. Like
95% of Emory nursing undergraduates, Flanagan relies on financial
assistance to cover his tuition. Help came through the Adopt-a-Scholar
Program, which paired him with nursing alumna and mentor Barbara
Reed.
“There are no words that can
express what Mrs. Barbara and the Reed family mean to me and my
loved ones,” said Flanagan.
“It is only fitting in this
blended world that we
provide compassionate nurses of varied backgrounds to help close
the culture gaps in our profession.”
That, he pointed out, would not be
possible
without the Adopt-a-Scholar Program and the Centennial Scholarship
Fund, established in honor of the nursing school’s 100th anniversary.
Proceeds provided by guests and sponsors at the Centennial Celebration
added some $80,000 to the $95,000 donated by nursing faculty, staff,
students, and alumni and organizations such as the Emory University
Women’s Club. The scholarship fund is now endowed, thanks
to the more than $230,000 raised thus far. Opportunities for contributing
to this fund remain so that it continues to grow.
As the evening concluded, Salmon asked
Flanagan and other students to stand for a toast
to them and their school.
“I began my remarks by asking
if you could imagine a world without nurses,” Salmon said.
“I’d like to end by asking you to imagine what the world
is going to be like with nurses like these. To the future!”
To
learn more about the Centennial Scholarship Fund, contact Kim Julian
at 404-727-6185, 877-676-0004 (toll free), or kjulian@emory.edu.
 |
|
| |
|
|
|
| |
|
|
|
 |
|
| |
|
|
| |
A
Family Affair

 he spirit of Nell Hodgson Woodruff, for whom the School of
Nursing is named, was ever present during a tea hosted by
her niece, Nell Woodruff Hodgson Watt, pictured here behind
the podium. Watt, known affectionately as “Little Nell,”
was all smiles as her daughter-in-law, Julie Watt, modeled
the nursing cape that Mrs. Woodruff wore as a longtime American
Red Cross volunteer and which Little Nell donated to the school
at the event. Edith Honeycutt, 39N, who is seated in the photo,
co-hosted the tea, a nursing school tradition begun by Mrs.
Woodruff during the 1940s. Honeycutt cared for four generations
of the Woodruff family, whose generosity propelled Emory to
the forefront of patient care, medical research, and university
education.
he spirit of Nell Hodgson Woodruff, for whom the School of
Nursing is named, was ever present during a tea hosted by
her niece, Nell Woodruff Hodgson Watt, pictured here behind
the podium. Watt, known affectionately as “Little Nell,”
was all smiles as her daughter-in-law, Julie Watt, modeled
the nursing cape that Mrs. Woodruff wore as a longtime American
Red Cross volunteer and which Little Nell donated to the school
at the event. Edith Honeycutt, 39N, who is seated in the photo,
co-hosted the tea, a nursing school tradition begun by Mrs.
Woodruff during the 1940s. Honeycutt cared for four generations
of the Woodruff family, whose generosity propelled Emory to
the forefront of patient care, medical research, and university
education. |
|
| |
|
|
|
 |
| |
|
|
|
| |
|
|
|

 |
|
The
Role of Faith in Health
Nursing,
theology offer new master’s program
 s
a yoga instructor Cheri s
a yoga instructor Cheri Mullen, 05N, is well versed in teaching students to calm and strengthen
their minds, bodies, and spirits. As a nurse, she finds it more
difficult to help patients in need of spiritual comfort.
Mullen, 05N, is well versed in teaching students to calm and strengthen
their minds, bodies, and spirits. As a nurse, she finds it more
difficult to help patients in need of spiritual comfort.
“When questions about God or
spirituality come up, we’re not sure exactly how to handle
it,” says Mullen, a staff nurse in the neurology unit at Emory
University Hospital.
A new master’s-level program
being offered by the School of Nursing and the Candler School of
Theology should provide answers and insight for Mullen and other
students in nursing, theology, and public health.
Darla Ura, clinical associate professor
in the nursing school, got the idea for the Faith and Health Program
a few years ago after completing coursework in parish and faith-based
nursing at the University of St. Louis. Armed with the initial concept,
she approached Dr. Karen Scheib, associate professor of pastoral
care and counseling at Candler, about establishing a joint certificate
program. Open to students of all faiths, the program will teach
them how to integrate faith traditions with health sciences. Students
also will learn how to advocate for social justice in religious
communities and society regarding issues of health and health care
and to create lasting partnerships between faith-based communities
and the health profession.
“Nurses’ roles have traditionally
focused on healing the body,” says Ura. “However, in
the past several years, there has been a growing realization of
the impact of spiritual and religious beliefs on healing and greater
emphasis on the holistic person. The Faith and Health Program provides
nurses the opportunity to expand their knowledge of faith practices
and the impact that religion and spirituality have in the healing
process of each patient.”
Nursing and theology faculty will
teach the program as students take required courses on faith and
health and elective courses, two of which must be outside their
own school. They will experience faith and health issues firsthand
through field work with different congregations.
“All religious traditions have
healing practices,” notes Scheib. “Since religion is
such an important fact of life in the United States, it is vital
that both religious professionals and health professionals understand
the way in which the faith of a person from any religious tradition
can hinder or help healing.”
To
learn more about the Faith and Health Program, contact the Office
of Admission at 404-727-7980, 877-676-0004 (toll free), or visit
the “Admission”
website. |
 |
| |
|
|
|
| |
|
|
|

|
|
Human
Resources for Health
Global
forum to address workforce shortage
 n
times of shortage, what can a nation’s health leaders do to
assure an adequate workforce to care for patients? Leaders from
around the world will journey to Atlanta in search of answers during
the next global forum hosted by the Lillian Carter Center for International
Nursing (LCCIN) this fall. n
times of shortage, what can a nation’s health leaders do to
assure an adequate workforce to care for patients? Leaders from
around the world will journey to Atlanta in search of answers during
the next global forum hosted by the Lillian Carter Center for International
Nursing (LCCIN) this fall.
The need for answers is compelling,
given that the ability of national health systems to provide safe,
reasonable, high-quality care is linked to the adequacy of the health
workforce. “Unfortunately, almost every country around the
world is experiencing significant challenges associated with shortages
of well-prepared health workers,” notes Dean Marla Salmon,
director of the LCCIN. “Governments worldwide are struggling
to address these shortages and are seeking strategies to assure
adequate supply, distribution, mix, and quality of health workers
in both the near and longer term.”
|
|
| |
|
|
 |
| |
|
|
| |
The
2006 forum, co-chaired by Salmon and Dr. Jeffrey Koplan, Emory’s
vice president for academic health affairs, will provide senior
government health leaders with new knowledge and insight to face
those challenges. It will build on the experiences of two previous
forums in which noted experts such as former President Jimmy Carter
and CDC director Dr. Julie Gerberding addressed the global nursing
shortage and emerging biological threats.
Like past forums, “The Breaking
Point: Human Resources for Health” will bring government chief
nursing officers (CNOs) and chief medical officers (CMOs) together
to collaborate on developing solutions. This time, they will gain
new insight on work conditions, trade policy, and health worker
migration to other countries.
Prior to the forum, CNOs and CMOs
will participate in a one-day workshop focusing on public health
response to health emergencies. The LCCIN also will host the Global
Government Chief Nursing Officers Institute, led by Salmon and Dr.
Anna Maslin of the Commonwealth Health Ministers Steering Committee
for Nursing and Midwifery. For CNOs only, the institute provides
a neutral and confidential setting for discussion of the challenges
they face. Previous topics of interest have included delivery of
health services in the face of workforce shortages, CNO roles, and
media strategies.
The
Global Government Chief Nursing Officers Institute, the Pre-Forum
Workshop, and the Global Government Health Partners Forum 2006 will
be held in Atlanta from October 29 to November 3. Participation
is by invitation only. For
information.
|
 |
| |
|
|
|
| |
|
|
|
 |
|
Science
and Women’s Health
Studies
look at diet, vitamin supplements
 re the latest results
re the latest results from the Women’s Health Initiative (WHI) surprising? Nursing
professor Dr. Ora Strickland says yes and no.
from the Women’s Health Initiative (WHI) surprising? Nursing
professor Dr. Ora Strickland says yes and no.
Primary findings from the Dietary
Modification Trial (DMT) of the WHI, the largest U.S. study ever
undertaken to improve the health of older women, were published
recently in the Journal of the American Medical Association
(February 8, 2006). Contrary to well-established evidence that a
reduced-fat diet helps prevent disease, the DMT showed that a diet
low in fat did not reduce the risk of colorectal cancer or significantly
reduce the risk of heart disease, stroke, or breast cancer.
The DMT promoted dietary change by
reducing daily fat intake to 20% and increasing vegetable and fruit
consumption to at least five servings and grains to at least six
servings. The study, comprising 48,835 postmenopausal women ages
50 to 79, found the following:
• Reducing fat did not reduce
the risk of colorectal cancer in postmenopausal women during 8.1
years of follow-up. However, questions remain about whether greater
adherence, longer intervention, or dietary change at an earlier
age would influence risks.
• The intervention did not significantly
reduce the risk of coronary heart disease, stroke, or cardiovascular
disease (CVD) in postmenopausal women. Only modest effects were
achieved on CVD risk factors, suggesting that more focused diet
and lifestyle interventions may be needed.
• During the same follow-up
period, a low-fat diet did not significantly reduce invasive breast
cancer risk in postmenopausal women. Breast cancer incidence was
9% lower for women in the dietary intervention group, compared with
those in the control group.
Strickland, who is a co-principal
investigator for the WHI site at Emory, says the results of the
diet trial were not as expected.
“We set a diet goal, in terms
of the percent of fat that should be in their diet, but as a group
the women never got down as low as 20%,” she explains. “The
results are based on an average fat intake that was higher than
what we recommended.”
Why was the goal so hard to
reach? “A diet very low in fat is harder to follow because
it’s not as tasty,” Strickland continues. “The
dieticians taught the women how to prepare food in a manner so it
would be more tasty, but can you really replace the good taste of
fat in some foods? Of course we wanted them to use more unsaturated
fat in their diets. And some of the women did lose weight. But reaching
a fat goal as low as 20% is difficult for a lot of people.”
The results of the DMT should not
be a signal for women to increase their fat intake and eat anything
they want, Strickland cautions. “Women still need to be very
concerned about the amount of fat in their diets as well as the
type of fat they consume. They need to have fat from vegetable sources
[such as olive oil] rather than animal sources.”
Results of another WHI study, the
Calcium and Vitamin D trial (CaD), were released in the New
England Journal of Medicine (February 16, 2006). This trial
tested whether supplementing diets with CaD would reduce the incidence
of bone fractures in postmenopausal women. Researchers also tested
whether supplementation would reduce the incidence of colorectal
cancer. After following 36,282 women, ages 50 to 79, for seven to
10 years, the trial found the following:
• A small improvement in hip
bone density was shown in healthy postmenopausal women, measuring
1.06% higher than the placebo group. However, the supplementation
did not significantly reduce hip fracture, and it also increased
the risk of kidney stones.
• Researchers also concluded
that daily CaD supplementation had no effect on the incidence of
invasive colorectal cancer among postmenopausal women.
Strickland cites two significant factors
regarding the CaD trial. Since this study began in the early 1990s,
researchers have learned that calcium, vitamin D, and magnesium
supplementation work better together than calcium and vitamin D,
the standard therapy at the time for preventing bone fractures in
older women. And, over time, the difference in the number of hip
fractures reduced may widen. “We haven’t studied the
women long enough yet,” Strickland notes.
Launched by the National Institutes
of Health in 1991, the WHI involved women at 40 U.S. sites, including
approximately 4,000 at Emory. The 15-year study looked at ways to
prevent coronary heart disease, breast and colorectal cancer, and
fractures from osteoporosis. Follow-up and spin-off studies related
to the WHI continue. |
 |
| |
|
|
|
| |
|
|
|
|
|
|









