













|
 |
| |
 |
|
 |
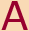 t
the end of fall semester, the nursing seniors in Lynette Wright’s
Human Clinical Genetics class team up in groups of three to present
posters on a host of genetic disorders. Naturally, the topics vary.
There’s 22q deletion syndrome, one of the most common causes
of learning disabilities and mental retardation; ectodermal dysplasia,
a group of 150 inherited disorders of the ectodermal tissue; neurologic
disorders such as Tourette syndrome and limb-girdle muscular dystrophy;
and many more. Among the common threads running through the students’
presentations is a discussion of the variety of genetic mechanisms
and a list of physical and behavioral symptoms that characterize
each genetic disorder and that students one day may observe in caring
for patients. t
the end of fall semester, the nursing seniors in Lynette Wright’s
Human Clinical Genetics class team up in groups of three to present
posters on a host of genetic disorders. Naturally, the topics vary.
There’s 22q deletion syndrome, one of the most common causes
of learning disabilities and mental retardation; ectodermal dysplasia,
a group of 150 inherited disorders of the ectodermal tissue; neurologic
disorders such as Tourette syndrome and limb-girdle muscular dystrophy;
and many more. Among the common threads running through the students’
presentations is a discussion of the variety of genetic mechanisms
and a list of physical and behavioral symptoms that characterize
each genetic disorder and that students one day may observe in caring
for patients.
Wright emphasizes the importance of
recognizing symptoms. Following the poster presentation on multiple
X and Y syndromes, she explains how body hair patterns in women
(triangular) and men (diamond-shaped) may signal a genetic disorder
if the gender and hair pattern are at odds. “Nursing is from
the neck up,” she tells the students. “It’s what
we observe and analyze when we’re looking at our patients.”
Whether her students know it or not,
Wright and Emory’s Nell Hodgson Woodruff School of Nursing
were into genetics long before it was cool. The school has offered
a genetics course for graduate students since 1979. And in 1997,
says Wright, the school became the first in the nation to require
all baccalaureate students to take a freestanding course in genetics
to better understand how this burgeoning science would affect their
work as nurses.
“We recognized early on that
no matter what area of nursing our students entered, whether neonatology,
intensive care, or geriatrics, their patients would be impacted
by genetics,” says Wright, who pioneered and leads the school’s
genetics teaching program. “As nurses, they would be on the
front lines of helping patients and family members understand and
deal with the genetic aspects of their diseases.” |
 |
| |
|
|
| |
 |
|
| |
 |
|
| |
Ahead
of the game |
|
| |
 right
and the school were ahead of their time. Last year, the credentialing
arm of the American Nurses Association adopted “Essential
Genetics and Genomics Nursing Competencies” guidelines developed
by an independent panel of nurse leaders from clinical, research,
and academic settings. The guidelines were endorsed by the International
Society of Nurses in Genetics, of which Wright is a founding member
and past president, and the National Coalition for Health Professional
Education in Genetics. The new guidelines spell out the “essential
genetic and genomic competencies for all nurses regardless
of level of academic preparation, practice setting, or specialty”
as well as the knowledge and skills needed to “prepare the
nursing workforce to deliver competent nursing care in the genomic
era of health care.” right
and the school were ahead of their time. Last year, the credentialing
arm of the American Nurses Association adopted “Essential
Genetics and Genomics Nursing Competencies” guidelines developed
by an independent panel of nurse leaders from clinical, research,
and academic settings. The guidelines were endorsed by the International
Society of Nurses in Genetics, of which Wright is a founding member
and past president, and the National Coalition for Health Professional
Education in Genetics. The new guidelines spell out the “essential
genetic and genomic competencies for all nurses regardless
of level of academic preparation, practice setting, or specialty”
as well as the knowledge and skills needed to “prepare the
nursing workforce to deliver competent nursing care in the genomic
era of health care.”
By the time these guidelines were
adopted, the School of Nursing had moved further down the genetics
road with the decision to require all master’s-degree clinical
program students, regardless of their specialization, to take the
“Genetics for Advanced Practice Nursing” course. Since
the class was created in 1979, also by Wright, more than 700 students
have passed through it on their way to advanced nursing practice.
But until spring 2006, it had been required only for master’s
students majoring in maternal and child health and nurse-midwifery.
Jane Mashburn, co-director of the
MSN program, says the decision to expand the course requirement
to all clinical master’s degree students was a no-brainer,
given the growing understanding of how genetic factors affect the
development and treatment of all diseases. That understanding is
also why she and other faculty members, both graduate and undergraduate,
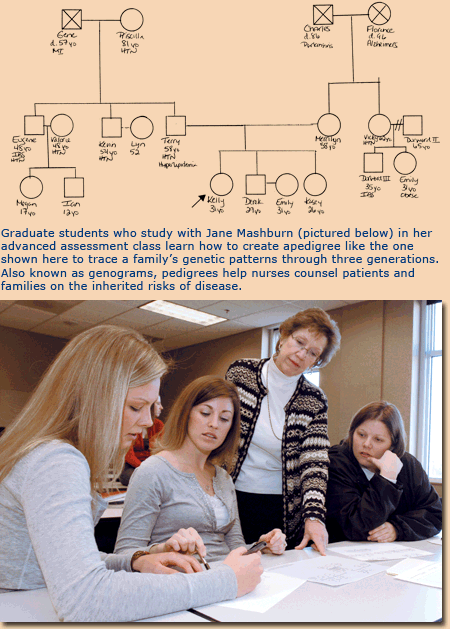
are expanding the genetic components in their own courses. Mashburn’s
class in advanced assessment, for example, now includes a segment
on making and understanding the significance of pedigrees (also
known as genograms) that trace genetic family patterns through three
generations. And the pharmacology course taught by Dr. Michael Neville,
clinical assistant professor in the Department of Adult and Elder
Health, now includes more pharmacogenetics, the study of genetic
factors that influence a person’s response to different drugs
and how to tailor drug treatments to individual genetic variations.
Including more genetics in nursing
education and research is as it should be, says Wright. “Genetics
is not something separate from the rest of nursing. It’s an
integral part of what nurses need to know.”
The genetic energy level in the school
rose late last spring when Wright, Mashburn, and Dr. Joyce King
organized a program on “The Genetics of Common Disorders:
Implications for Curricula and Practice” for faculty from
the School of Nursing and the physician assistant program in the
School of Medicine. The program updated the faculty on genetic understanding
of diabetes, cancer, and micro-deletion syndromes (caused by a chromosomal
deletion and causing problems ranging from short stature and cleft
palate to emotional and behavioral issues). King spoke about her
research into the genetics of obesity and joined other nursing faculty
to chair sections on pharmacogenetics and the public health implications
of the Human Genome Project. Faculty from the medical school’s
Department of Human Genetics shared their expertise on diagnostic
and therapeutic advances for genetic disorders, including schizophrenia,
cancer, and liposomal storage diseases (in which a missing or faulty
gene prevents metabolism of certain food products). Dr. Neil Lamb,
assistant professor of human genetics, gave the keynote address,
aptly titled “Researching the Genetics of Common Disorders:
Why It Will Take Us All.”
The participation of faculty members
from the Department of Human Genetics is emblematic, says Wright,
of the growing partnership between the schools of nursing and medicine.
She doesn’t find that surprising. Three years earlier, shortly
before more than 80 nursing seniors were set to begin her required
genetics course, Wright was grounded temporarily by back surgery.
Human Genetics chair Stephen Warren and other faculty from that
department stepped in and taught the nursing students each week
for the semester.
The driving force behind such cooperation
is the belief shared by health care providers across the Woodruff
Health Sciences Center that genetics education is indispensable
for today’s health care providers, including nurses. It also
may have helped that the medical school saw their ailing nursing
colleague as a longstanding member of an interdisciplinary genetics
club. |
|
| |
|
|
| |
 |
|
| |
|
|
| |
Welcome
to Club Genetics |
|
| |
 hen
Wright arrived at the School of Nursing in 1974 to enter the master’s
clinical specialist program in pediatrics, she wanted to learn more
about what caused the birth defects she saw as a pediatric nurse.
Since the nursing school had no course in genetics, Wright persuaded
the late Dean Ada Fort to allow her to cross a then-deep chasm to
take a genetics seminar in the medical school. Fort was dubious
that a nursing graduate student needed to do that. Dr.
Louis (Skip) Elsas, then head of the medical genetics program, was
equally dubious that she could. Wright had no formal background
in genetics. Nonetheless, Elsas let her join the young MD and PhD
students in the class, sink or swim. hen
Wright arrived at the School of Nursing in 1974 to enter the master’s
clinical specialist program in pediatrics, she wanted to learn more
about what caused the birth defects she saw as a pediatric nurse.
Since the nursing school had no course in genetics, Wright persuaded
the late Dean Ada Fort to allow her to cross a then-deep chasm to
take a genetics seminar in the medical school. Fort was dubious
that a nursing graduate student needed to do that. Dr.
Louis (Skip) Elsas, then head of the medical genetics program, was
equally dubious that she could. Wright had no formal background
in genetics. Nonetheless, Elsas let her join the young MD and PhD
students in the class, sink or swim.
Wright thought it might be sink at
first. She didn’t even recognize the scientific language that
faculty and other students were speaking. But gradually she realized
that her training and experience as a nurse brought something real
and valuable to the seminar table. She came to class not knowing
much about genetics, while her medical school classmates often came
not knowing much about patients. “We learned a lot from each
other,” says Wright. At the end of the course, she was asked
to join the medical genetics program. “They knew they wanted
me, but they didn’t quite know what to do with me,”
she recalls, so they trained her alongside their medical residents
and let her develop her role as a clinical nurse specialist in genetics.
The 1970s was a heady time in that
field, as scientists increasingly understood the power of a single
gene in causing rare but disastrous disorders. Phenylketonuria (PKU),
a recessive genetic disorder, was a perfect example. One in 1,400
babies inherit from both parents a defective gene for the metabolism
of phenylalanine, the protein in most foods, including breast milk.
Without treatment, metabolites from an ordinary diet build up in
the infant’s brain, causing progressive and irreversible retardation
and other problems. But such metabolic disorders are easily detected
shortly after birth, and parents can make dietary changes to prevent
such a buildup. It’s not a simple or short-term task, but
treated children grow up healthy and bright, a happy testimony to
the power of genetic testing and therapeutic intervention.
Medical geneticists at Emory established
Georgia’s heel-stick screening program for PKU, and Emory
medical genetics became the referral center for babies found to
have the genetic disorder. Wright counseled patients and families
and did much of the hands-on work to expand Georgia’s newborn
screening program from one to eight metabolic genetic diseases (it
will soon expand to about 30). Some of the outreach clinics she
helped establish across the state still operate today, helping support
more than 5,000 patients with genetic disorders and followed by
Emory clinicians. When the American Board of Medical Genetics first
offered certification in genetic counseling, Wright was one of the
first two nurses from Georgia to earn it. The other was Karlene
Coleman, also an Emory nursing graduate and the first person mentored
by Wright, who today serves as a genetics counselor with Children’s
Healthcare of Atlanta. (See “Leader of the
Pack”.)
From the moment Wright completed her
master’s degree in 1974, she was on a mission—now in
its 32nd year—to bring more genetics into nursing education.
At first, she was a frequent guest lecturer at the school, sharing
some of what she did and saw at work. In 1977, she began offering
the genetics course that eventually became mandatory for all master’s
students in maternal and child health and nurse-midwifery. As this
graduate course grew in popularity, she found an ally in Dr. Helen
O’Shea, then-director of the baccalaureate program, who was
eager to see all undergraduates exposed to more genetics. Since
Wright’s undergraduate course was first offered almost a decade
ago, every baccalaureate graduate of the nursing school has been
prepared to recognize and deal with the genetic issues that nurses
increasingly face in practice.
The course has evolved over the years,
says Wright, along with the field of genetics itself. In the late
1970s, graduate students studied Mendelian patterns of inheritance
and how to collect family histories. As genetics became more complex,
students learned about the multifactorial nature of most diseases,
including cancer, heart disease, juvenile and adult-onset diabetes,
asthma, allergies, and autoimmune diseases such as rheumatoid arthritis.
In cancer genetics, for example, students learned about the genes
that turn on tumor formation (oncogenes) and the tumor-suppressor
genes that tried to turn it off. They learned about inherited risk
of breast, colon, ovarian, and other cancers and the promise and
problems of genetic testing for these and other diseases. The course
changed yet again when the deciphering of the human genome, the
body’s entire genetic blueprint, improved scientists’
ability to recognize complex, sometimes subtle genetic disorders
and determine the genetic variations that predispose individuals
to develop human disease, perhaps in conjunction with environmental
or behavioral factors.
But some things have remained constant
over these three decades. First is the emphasis on the roles and
responsibilities of nurses in terms of recognizing genetic problems,
making certain interventions are begun as early as possible, knowing
how to make appropriate referrals, carrying out therapies, providing
initial and ongoing support, preparing patients for specialized
testing, and providing follow-up and ongoing care. “We don’t
want to make them geneticists,” says Wright. “We want
to make them better nurses.”
Second is an emphasis on the patient.
Wright considers herself a translator of complex science into real-world
information, placing it in the context of cases and showing how
it applies to all areas of nursing. Her courses also provide information,
as called for in the new national genetics and genomics nursing
competencies guidelines, on how nurses can tailor genetic information
and services to clients based on their culture, knowledge level,
religious beliefs, and other factors.
Third is an emphasis on lifelong learning.
Genetics is never going to stand still, says Wright. Consequently,
she never teaches her classes, undergraduate or graduate, in “information-in/information-out”
style. Students use the Internet and emerging learning technology
both to learn facts and to learn how to learn, so they will have
the resources they need to stay current throughout their professional
lives. (See “A Genetics Primer” for
a handful of resources that students and faculty find helpful.) |
|
| |
|
|
| |
 |
|
| |
|
|
|
| |
 |
|
 |
| |
 |
|
 |
Leader
of the Pack |
 |
 |
 arlene
Coleman, 75MN, is a certified genetics counselor at Children’s
Healthcare of Atlanta at Egleston. Deeply committed to interweaving
genetics with nursing education, Coleman lectures on genetics
at Emory’s medical and nursing schools and serves as
a preceptor several times a year for students from the School
of Nursing who want more hands-on experience in genetics before
entering practice. “I’m lucky,” Coleman
says, “to be involved with two incredibly forward-looking
institutions—Children’s, which staffs its hospitals
with genetics counselors, and the School of Nursing, which
is ahead of the curve in recognizing the importance of genetics
training to nurses.” arlene
Coleman, 75MN, is a certified genetics counselor at Children’s
Healthcare of Atlanta at Egleston. Deeply committed to interweaving
genetics with nursing education, Coleman lectures on genetics
at Emory’s medical and nursing schools and serves as
a preceptor several times a year for students from the School
of Nursing who want more hands-on experience in genetics before
entering practice. “I’m lucky,” Coleman
says, “to be involved with two incredibly forward-looking
institutions—Children’s, which staffs its hospitals
with genetics counselors, and the School of Nursing, which
is ahead of the curve in recognizing the importance of genetics
training to nurses.”
Coleman believes her training
as a nurse—her clinical knowledge and experience, her
understanding about how to navigate the complex health care
system, and her ability to hear and respond to patients—has
been invaluable to her career and to her young patients and
their families. “More nurses should consider entering
genetics counseling,” she says, “where they are
so badly needed. But no matter what direction nurses take
their training, genetics will lie at the heart of it.”
She is encouraging the school to consider offering a master’s
degree in genetics because of the need and the opportunity
for nurses with such training.—Sylvia
Wrobel |
 |
| |
 |
|
|
|
| |
|
|
| |
On
the front lines |
|
| |
 r.
Paul Fernhoff first met Wright when she worked in the medical school
in the 1970s. He considers her “one of the pioneers in understanding
the power of genetics and how it would influence health care in
the 21st century, including nursing.” r.
Paul Fernhoff first met Wright when she worked in the medical school
in the 1970s. He considers her “one of the pioneers in understanding
the power of genetics and how it would influence health care in
the 21st century, including nursing.”
Speaking for his medical colleagues,
Fern-hoff applauds Wright’s determination to infuse the next
generation of nurses with this knowledge and understanding. As the
head of clinical genetics in the Division of Medical Genetics, he
sees firsthand the genetics-related roles nurses play in hospitals,
clinical offices, public health programs, and elsewhere. When abnormal
results come back from newborn screening, for example, someone from
the local health care provider’s office notifies the parents
and asks them to come into one of the genetics clinics for follow-up.
More often than not, says Fernhoff, it’s a nurse who makes
that difficult call and who must deal with the questions and concerns
of the family in the days ahead. No matter what the disease or disorder,
he adds, nurses often are the frontline health professionals who
help patients and their families understand the genetic and familial
implications of the diagnosis and treatment. As genetics gains greater
predictive power and becomes increasingly incorporated into daily
health care, it will be more imperative that all nurses have a strong
genetics basis.
Judging by the enthusiasm of School
of Nursing faculty—the vast majority of whom responded to
last spring’s program with plans to expand the genetics components
of their own courses—and feedback from graduates who say that
studying genetics better prepared them as nurses, Emory nursing
students will stand ready on the front lines, wherever they practice.
Sylvia Wrobel is former associate
vice president for health sciences communications and a frequent
contributor to Emory’s health sciences publications. |
|
| |
|
|
|
|
|
| |
|
|
| |
|
|
|
|
|









