






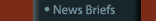






|

|
 |
 r.
Maureen Kelley’s passport reads like a mini-guidebook to the
Caribbean, with the stamps of St. Vincent, Trinidad, Jamaica, and
Suriname peppering its pages. Then there are the distinctive marks
of Ethiopia and Russia—destinations to which Kelley expects
to soon return. r.
Maureen Kelley’s passport reads like a mini-guidebook to the
Caribbean, with the stamps of St. Vincent, Trinidad, Jamaica, and
Suriname peppering its pages. Then there are the distinctive marks
of Ethiopia and Russia—destinations to which Kelley expects
to soon return.
While Kelley’s trips crisscross
the globe, they share a similar theme—helping nurses and nurse
midwives strengthen their education and practice and decrease maternal
and infant mortality rates in their respective countries.
As the newly named holder of the Independence
Chair in Nursing, chair of the Department of Family and Community
Nursing, and a nurse-midwife at Emory Crawford Long Hospital (she
was the hospital’s first midwife in 1983), Kelley is known
by many for her dedication to family health. “Maureen is regarded
by students and colleagues in much the way you would want your midwife
to be: calm, kind, and completely nonjudgmental,” says nursing
doctoral student Maeve Howett, 82C, 85N, 97MSN.
The focus of the School of Nursing
on improving the health of vulnerable people worldwide has only
deepened Kelley’s dedication to maternal and infant health.
Her travels have allowed her to see the disparities among countries
that are desperately short of resources. But they also have provided
great opportunities for sharing the common ground that links nurses
and midwives the world over.
“There is this bond we all have—I
love this about midwives—we can be anywhere in the world and
share and tell stories and compare clinical situations,” she
says. “We use storytelling as a means of communication and
connection—connection to our commitment to be ‘with
women’ (the literal meaning of ‘midwife’) and
communication of our own pregnancy and birth experiences, which
are universal.”
Through her travels, Kelley has gathered
a diverse collection of compelling stories. “In Ethiopia,
a traditional birth attendant proudly shared her birth log and talked
about her commitment to the women of the village and how she handled
medical complications,” she recalls. “In Moscow, the
midwives told stories of their support for women who breastfeed
and their desire to have continuity of care. In Jamaica, community
nurses (who serve as midwives) toured us through their health center
and described their outreach to teens. They live next door to the
clinic and know everyone in the community.
“The other gift of midwifery
is that we share a miraculous experience with families—birth.”
These stories were among those shared
during the International Confederation of Midwives (ICM) Americas
Regional Conference in Trinidad last spring, which Kelley attended.
The meeting brought together 400 nurse-midwives from North America,
South America, and the Caribbean. During the meeting, Kelley co-led
two educational workshops, helping mark the first time that educators
from the Americas sat down together to discuss topics of common
interest.
 Kelley
also took part in the Young Midwifery Leaders Program, an ICM initiative
involving young nurse Kelley
also took part in the Young Midwifery Leaders Program, an ICM initiative
involving young nurse
mid-wives from Germany, Kenya, South Africa, Slovakia, and Trinidad.
Each country nominated one nurse midwife under age 35 and one mentor
to attend the meeting. These select young leaders are participating
with their mentors in a three-year program to strengthen their midwifery
education, knowledge, and leadership skills.
The importance of such gatherings
can’t be underestimated. “Around the world, the word
‘midwife’ can mean different things—a community
member who learned from her mother or
grandmother, somebody with a nursing degree, or someone with a PhD,”
says Kelley. “This variation can lead to different interpretations
about the role of the midwife in maternal and child health. It’s
important for the public and the medical community to understand
that the midwife’s role varies according to the traditions
and educational requirements in different countries. Midwives can
and do play a key role in pregnancy and birth globally and are critical
to the success of
safe motherhood.
“Midwives also strive to understand
the global picture of maternal and child health and how they can
serve as advocates,” she continues. “They also need
to understand the larger context: Where does nursing and midwifery
fit in your country, how do you advocate for women, how do you get
to the table [where decisions are made] so you can function as an
advocate? Maternal mortality is a huge problem in many of these
countries. How do midwives help impact that?”
Strong
ties to the Caribbean
  lways
a teacher, Kelley believes that standardization and competency-based
education are key to lways
a teacher, Kelley believes that standardization and competency-based
education are key to
optimizing midwives’ success in improving care for mothers
and babies. Toward that end, she is working with the Caribbean Community
and Common Market (CARICOM) to address this issue. Last spring,
Kelley traveled to Suriname as an observer of the meeting of the
Regional Nursing Body—comprised of chief nursing officers
from CARICOM-member countries—to investigate the feasibility
of developing core competencies for nurse-midwives across all Caribbean
countries.
The task is not as formidable as it
seems. Caribbean nurses in separate nations already share standardized
licensure requirements and a common licensing examination (which,
incidentally, the United States does not share with other nations).
“The challenge is standardization of core educational competencies.
You don’t want differing outcome expectations, which would
lead to a nine-month midwife program in one country and a three-year
program in another,” Kelley explains. “The goal in the
next two years is to develop standard educational competencies that
each country agrees upon.”
Her ties to the Caribbean were strengthened
last March when she co-led a group of undergraduate and graduate
nursing students to Jamaica to assist in hospitals and clinics.
The trip was one of three spring break alternatives funded by the
O.C. Hubert Charitable Trust for students with a special interest
in faith, international health, and vulnerable populations (see
“Spring Break Alternative” in the News Briefs section).
Kelley accompanied her students to Montego Bay, where they assisted
nurses in an HIV/AIDS clinic, a pediatric hospital wing, and community
mental health programs.
“I was very proud of our students,”
she says. “At the end of each day, the students came home
with stories about their experiences, and we spent more than two
hours debriefing about what they had seen and observed. The respect
they had for everyone they encountered was wonderful. They were
willing to examine issues from different viewpoints and help each
other explore important issues of faith and health and their integration
into their personal and professional lives.”
Mothers
and Babies in Moscow
 hile
plans are in the works for a similar trip to Jamaica in 2005, Kelley
is planning yet another international foray next spring—her
second visit to a hospital outside of Moscow to collaborate with
colleagues on improving the reproductive health of women in Russia.
The birth rate there has declined dramatically, and high infant
and maternal mortality rates have prompted President Vladimir Putin
to declare a crisis. hile
plans are in the works for a similar trip to Jamaica in 2005, Kelley
is planning yet another international foray next spring—her
second visit to a hospital outside of Moscow to collaborate with
colleagues on improving the reproductive health of women in Russia.
The birth rate there has declined dramatically, and high infant
and maternal mortality rates have prompted President Vladimir Putin
to declare a crisis.
The medical community has responded.
Kelley is part of the Balashikha Project, a collaborative program
involving the Future  of
Russia Foundation (FRF), the World Health Organization/Collaborating
Center, the Centers for Disease Control and Prevention, and Emory’s
School of Medicine and funded by the FRF, Rotary Atlanta, and Rotary
International. She joins Emory perinatal and neonatal health specialists
Alfred Brann and William Sexson and neonatal nurse practitioner
Janet Thigpen in the effort to improve maternal health in Russia.
This past fall, Russian health care providers visited Atlanta for
the third time to exchange ideas and experiences with doctors, nurses,
and midwives here. of
Russia Foundation (FRF), the World Health Organization/Collaborating
Center, the Centers for Disease Control and Prevention, and Emory’s
School of Medicine and funded by the FRF, Rotary Atlanta, and Rotary
International. She joins Emory perinatal and neonatal health specialists
Alfred Brann and William Sexson and neonatal nurse practitioner
Janet Thigpen in the effort to improve maternal health in Russia.
This past fall, Russian health care providers visited Atlanta for
the third time to exchange ideas and experiences with doctors, nurses,
and midwives here.
Through the five-year Balashikha Project,
health experts have created a perinatal center within a hospital
in Balashikha, made it a referral center for high-risk mothers and
babies in the Moscow region, and begun to develop a perinatal surveillance
system. The project is now in its third year.
“Maureen has been 
instrumental in working with her Russian colleagues to customize
the partogram [a graphic recording system] to monitor the status
of the mother and fetus during labor,” says Brann. “She
is also advocating for greater emphasis on
family-centered maternity
care and prenatal education.”
“The project is ensuring at
least that the babies being born are going to survive intact,”
he adds. “Maureen’s nurse-midwifery assessment and evaluation
skills are critical to changing those practices.”
Many challenges lie ahead. The physical
facility is being upgraded and new equipment added. Human resources
are strained. Family participation in labor and birth is not yet
part of the system. Once the immediate issues of monitoring and
improving the health of mothers and newborns are addressed, Kelley
and her Russian colleagues want to focus more on how care is delivered.
“We hope to make it as family-centered as possible,”
she says.
That’s a given for those who
know her, says Brann, who worked with Kelley at the University of
Mississippi Medical Center in the 1970s. “She’s an excellent
clinician and a compassionate woman who delivers superb care.”
Rebecca
Rakoczy is an Atlanta freelance writer and former editor of Pulse,
a monthly nursing supplement published by The Atlanta Journal-Constitution.
|


 |
| |
|
|
|
|
|







