












|
| |
|
|
 |
| |
|
|
 |
Timeline
continued from A Marriage Made in Atlanta |
 |
| |
|
|
 |
 |
Cardiologist
Nanette Wenger was appointed
director of the cardiac clinics at Grady Hospital. She
would go on to become a leading expert in heart disease
in women. |
 |
| |
|
|
 |
 |
Charles
R. Hatcher
performed Georgia’s first “blue baby”
operation using open heart surgery. The next year, he
performed Georgia’s first aortic valve replacement.
Successful double and triple valve replacements followed
soon thereafter. He built the heart surgery program
at Emory into one of the nation’s largest and
most successful, before becoming director of The Emory
Clinic in 1976. He later served as director of the Woodruff
Health Sciencs Center from 1984 to 1993. |
 |
 |
 |
Hamilton
Holmes became
Emory’s first African-American medical student.
He became an orthopedic surgeon and eventually was medical
director of Grady Hospital. Today, each medical school
class is half and half men and women and about 30%of
students are minorities. |
 |
 |
 |
Asa
Yancey,
a former medical director of Hughes Spalding Pavilion
of Grady Hospital, was the first African-American member
of the medical faculty. Yancey was medical director
from 1972 to 1989. His son Arthur is on Emory’s
faculty today. |
 |
 |
 |
The
Robert W. Woodruff Medical Center (later renamed The
Robert W. Woodruff Health Sciences Center) was
established. Also, doctors at Emory Hospital performed
Georgia’s first intrauterine transfusion to save
the life of a fetus threatened by Rh negative blood
reaction. And Geogria’s first coronary arteriogram
was done by Robert Schlant at Grady Memorial Hospital.
This same year, Garland Perdue performed Georgia’s
first kidney transplant. |
 |
 |
 |
Charles
Hatcher performed Georgia’s first successful coronary
bypass surgery, at Emory Hospital. |
 |
 |
 |
A
$25-million expansion plan for Crawford Long Hospital
was announced, including a nine-floor addition. |
 |
 |
 |
Emory
Hospital began a $30 million addition to patient care
and teaching facilities, which was completed in 1978. |
 |
 |
| |
John
Stone founded Emory’s residency program in emergency
medicine. |
 |
 |
 |
Andres
Gruentzig
first performed angioplasty in Zurich, Switzerland.
He joined the Emory faculty in 1980 and continued to
perfect the procedure that helped shape interventional
cardiology and changed forever the treatment of atherosclerosis.
He died in a plane crash in 1985. |
 |
 |
 |
Ralph
Vogler performed
Emory’s first bone marrow transplant on a patient
with acute leukemia.
This same year, Emory University received approximately
$105 million from the Emily and Ernest Woodruff Fund,
the largest gift given in an educational institution
in US history and the lead gift in the $160 million
campaign to support scholarships, teaching, research,
and building projects across the university, including
the School of Medicine. |
 |
 |
 |
James
F. Glenn became
dean, serving till 1983.
This same year, The National Eye Institute selected
Emory to direct the prospective evaluation of radial
keratotomy study, the largest and most comprehensive
clinical investigation of this procedure to correct
myopia. |
 |
 |
 |
Emory
doctors injected a thrombolytic agent into the coronary
artery of a patient to stop a heart attack, the first
use of this treatment in Georgia. |
 |
 |
 |
George
Brumley,
then chair of pediatrics, served as interim dean till
1984. |
 |
 |
 |
Richard
Krause
was recruited from the NIH to become dean, serving till
1988. His mandate was to build Emory’s reputation
in research to be on a par with that in teaching and
patient care. |
 |
 |
 |
Surgeons
at Emory performed Atlanta’s first heart
transplant.
This same year, Robert Woodruff, 95, died on March 7
at Emory University Hospital. During his lifetime, he
gave away an estimated $350 million, which included
$230 million to Emory University. |
 |
 |
 |
Luella
Klein
became the first female chair of a department (gynecology
and obstetrics) at Emory, serving till 1992. She also
served as the first female president of the American
College of Obstetricians and Gynecologists.
This same year, Atlanta industrialist O.
Wayne Rollins donated $10 million for construction
of the Rollins Research
Center. This new building doubled research space at
Emory and helped set the stage for Emory researchers
tp apply for and receive millions of dollars in research
grants. |
 |

 |
 |
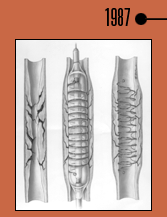
John
Douglas and colleagues performed the first coronary
stent
implant in the United States. This same year,
Emory doctors inserted the first implantable defibrillator
in a patient in Georgia.
Also in 1987, Emory doctors performed the state’s
first liver transplant. |
 |

 |
 |
Emory
doctors performed Georgia’s first directional
atherectomy to scrape and remove plaque from arterial
walls. Also this year, Emory surgeon Kirk Kanter performed
the state’s first pediatric heart transplant on
a 3-year-old at Egleston Hospital.
Timeline continued on The
Money Trail |
 |
| |
|
|
|
|
 |
 |
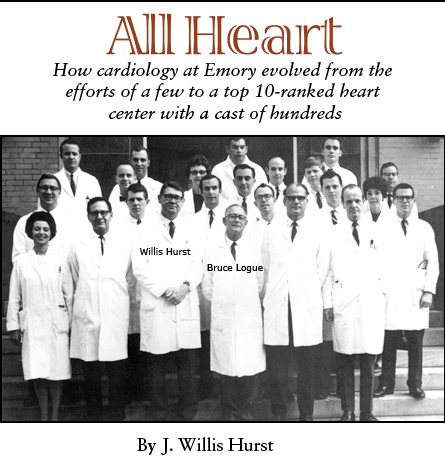
Editor’s
note: J.
Willis Hurst needs no introduction. Cardiologist to President Lyndon
B. Johnson, creator of the most influential textbook on the heart,
founding member of The Emory Clinic, longtime chairman of medicine,
and award-winning teacher, Hurst, at 83, still spends his days teaching
house officers and medical students and writing prolifically. His
recent “What Do Good Doctors Try to Do?”in the Archives
of Internal Medicine is one of his most popular articles to date.
When we asked Hurst to contribute an article to Emory Medicine on
a brief history of cardiology at the School of Medicine, he graciously
composed a 26-page manuscript. It took that many pages to do justice
to the history, he explained. We’ve touched the highlights
of his story here, but for the complete version, which includes
names and activities, see: allheart.html
|
 |
| |
|
|
 |
I
am sometimes asked why Emory cardiology is consistently ranked in
the top 10 of the nation’s best heart centers. Here is the
story.
Note that the story, involving patient care, excellent teaching,
and ground-breaking clinical and basic research, wouldn’t
exist without the contributions of Emory faculty members in many
departments, including medicine, pediatrics, cardiac surgery, vascular
surgery, radiology, anesthesiology, physiology, and pharmacology,
as well as the nursing staff. Likewise, the story unfolds in many
settings: Emory University Hospital, Grady Memorial Hospital, Atlanta
Veteran’s Affairs Medical Center (VAMC), Emory Crawford Long
Hospital, Egleston Children’s Hospital, The Emory Clinic,
dozens of satellite locations, and several research buildings. |
 |
| |
|
|
 |
Our
story begins in the 1940s. In 1942, Eugene Stead became Emory’s
first full-time chairman of the Department of Medicine. He, Jim
Warren, and others developed a cardiac catheterization laboratory
at Grady Hospital––only the third such laboratory in
the world. Warren performed the first cardiac catheterization for
diagnostic purposes in 1946.
Stead recruited Bruce Logue, a man of vision, a superb clinician,a
charismatic teacher, and an excellent writer. Logue had the right
combination of abilities to develop a comprehensive cardiology center
here. He was the founding father of the Georgia affiliate of the
American Heart Association.
I joined the faculty to work with Logue in 1950. When Paul Beeson
was chairman of the Department of Medicine, my job was to teach
house staff and fellows at Emory Hospital and Grady. I was charged
with helping build a consulting referral practice, with a mandate
also to engage in clinical research and to write.
In 1951, I urged our two cardiac surgeons to operate on one of my
patients who had severe mitral valve stenosis. They did so. It was
probably the first operation of that type to be performed in the
South.
Because pediatric cardiology was not yet a discipline, Logue and
I also served as pediatric cardiologists. I worked with a cardiac
fellow to develop a new, standardized preparation of digitalis for
children, which continues to be used today.
Logue and I were founding members of the Emory Clinic, which was
formed in 1953 by the merger of the Private Diagnostic Clinic and
several other units in Emory Hospital. This development was of utmost
importance because it created a superb method for growth and financial
support.
A few years later, at the age of 35, I was appointed as chairman
of the Department of Medicine. I began my new job in February 1957,
at the age of 36, and didn’t leave the chairmanship until
1986. It came about like this: I was drafted by the US Army for
the second time in 1955. During my year’s absence from Emory,
the chairmen of medicine, surgery, and obstetrics became embroiled
in a disagreement with Dean Arthur Richardson, ultimately leading
to their release. Becoming chairman of the department gave me new
opportunities. Accordingly, for the next 30 years, I made every
effort to develop all of the divisions of the department. |
 |
 |
 |
By
1957, the story of Emory cardiology had progressed to include three
cardiologists at Emory University Hospital and one at Grady Memorial
Hospital. No research space and no hard-core budget for the Department
of Medicine yet existed. The National Heart, Lung, and Blood Institute
gave a $25,000 annual stipend to every medical school in the nation
for the teaching of cardiology. But we obviously needed more than
that to support our programs. We needed many more talented people,
research space, and a budget.
An important financial commitment by the Robert W. Woodruff Foundation
allowed us to build new cardiac laboratories within the new Grady
Hospital facilities, completed in 1958. Also, in that year, the
Crippled Children’s Service of Georgia donated funds to build
a cardiac catheterization laboratory in the relatively new Woodruff
Research Building, which was attached to Emory Hospital and became
the first cardiac catheterization laboratory located in a private
hospital in Atlanta.
Each year, Emory offered the only postgraduate courses in cardiology
in the Southeast. We invited national and internationally known
experts to help present the courses. Hundreds of practicing physicians
attended the courses, and Emory became recognized around the world
as a major teaching center for cardiology. We organized the first
postgraduate course in cardiology for the American Heart Association
in 1963, followed a year later with the first postgraduate course
in cardiology for nurses. The internationally known speakers and
the participants of the courses learned what was happening at Emory,
and I am pleased to say, they liked what they saw.
I created the textbook, The Heart, with Logue in the early
1960s. The book brought further acclaim to our cardiology efforts.
It was becoming clear that textbooks in cardiology needed redoing.
When single individuals were writing them, they took too long to
finish. The first chapter would be out of date by the time the last
chapter was done. So I came up with the notion of a multi-authored
book. With significant contributions from Robert Schlant (director
of cardiology from 1962–1986), Nanette Wenger (today well-known
for her study of heart disease in women and chief of cardiology
at Grady), and others, the first edition of The Heart was published
in 1966. Subsequently, a new edition was created every four years.
With its translation into six languages and currently in its tenth
edition, it has brought international recognition to Emory cardiology.
After the seventh edition, I passed the editor-in-chief responsibilities
to Schlant and Wayne Alexander, the current chairman of the Department
of Medicine, at which time the publishers renamed the book Hurst’s
The Heart. Although there are many books on cardiology today, the
Emory book continues to be popular and used worldwide.
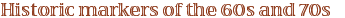
Several other pioneering developments accompanied the decade of
the 1960s. Emory physicians at Grady were the first in Atlanta to
use cardiac defibrillation for the treatment of atrial fibrillation
and to use a cardiac pacemaker. Schlant performed the first coronary
arteriogram in Atlanta in the Grady cardiac laboratory. Robert Franch,
working in the cardiac catheterization laboratory on the Emory campus,
performed the first atrial septotomy in the South in 1967.
Two additional divisions to the Department of Medicine brought faculty
members with cardiovascular orientations to Emory. Leon Goldberg,
for example, who became director of clinical pharmacology, quickly
catapulted his division of experts in cardiovascular drugs to national
recognition. A division of clinical physiology was added to the
department of medicine to emphasize the use of basic science principles
in the clinical training of students and house officers.
At Egleston, Catherine Edwards and Dorothy Brinsfield were laying
the ground work for what was to become a nationally known pediatric
heart center. William Plauth was appointed director of pediatric
cardiology and developed the first cardiac catheterization laboratory
at Egleston in 1975.
The arrival of Charles Hatcher to the Division of Cardiothoracic
Surgery during the early sixties adds another chapter to our story.
By 1971, Hatcher was director of the division, and his leadership
was a major force in the development of cardiac surgery at Emory.
Emory cardiac surgeons became leaders in coronary bypass surgery,
with patients being referred from other states and other countries.
Hatcher continued as division director until 1995, also serving
as director of The Emory Clinic from 1976–1984 and leading
the Woodruff Health Sciences Center from 1984–1996.
Robert Guyton became director of the Division of Cardiothoracic
Surgery and propelled the division to the top ranks. In the meantime,
Robert Smith was developing a peripheral vascular disease service
at Emory Hospital. His team became noted for their low operative
risk, and Smith was among the first in the country to operate on
the carotid artery using only local anesthesia. |
 |
 |
 |
| |
|
 |
 |
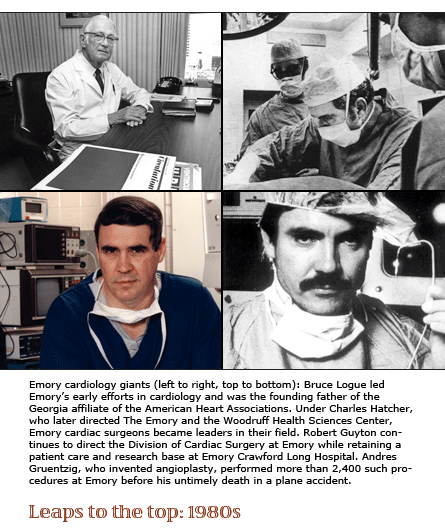 |
 |
The
year 1980 marked a milestone in our history. Bruce Logue retired
from his duties at Emory Hospital and The Emory Clinic and became
director of the Carlyle Fraser Heart Center at Crawford Long Hospital.
The center, created in 1976 thanks to the generosity of the Fraser
family, thrived under Logue’s leadership.
The same year brought Andreas Gruentzig to the Emory faculty. Just
three years before at a hospital in Zurich, Switzerland, Gruentzig
made history by inserting a catheter into a patient’s clogged
coronary artery and inflating a tiny balloon. The procedure restored
blood flow to the heart, and angioplasty was invented. Through his
acquaintance with Spencer King, John Douglas, and others at Emory,
I recruited Gruentzig to join our team. I originally gave him adequate
office space in the connector between 4E and 4G in Emory Hospital.
Later I added an entire floor in the connector for his use, one-half
of the entire space allotted to the Department of Medicine.
Gruentzig was a genius. While he loved life and lived on “the
edge,” he was a tender, honest, and compassionate advocate
for his patients. During his five years at Emory–before he
and his wife were killed in a tragic plane accident–he performed
more than 2,400 coronary angioplasties, sponsored an annual postgraduate
course attended by hundreds, and propelled cardiology at Emory to
the top ranks of world medicine.
In the 1980s, the amount of clinical research at Emory had reached
the point that a fulltime statistician was needed to assess our
results. Meanwhile, the cardiac surgery program was keeping pace.
The first cardiac transplant performed at Emory Hospital came in
1985, followed by the first transplant in children at Egleston in
1988. Quite simply, the transplant service became recognized as
one of the best in the country. |
 |
 |
 |
After
serving as chairman of the Department of Medicine for 30 years,
I retired from that position in November of 1986. I passed the reins
to Juha Kokko, who appointed Wayne Alexander to lead the division
of cardiology in 1988.
Alexander, who holds the R. Bruce Logue professorship, is an internationally
known cardiologist and is recognized as one of the greatest department
chairmen in the nation. He greatly expanded the cardiology research
effort at Emory. During his tenure, a large amount of research space
has become available in the greatly enlarged Woodruff Research Building.
Several cardiac catheterization laboratories, a new electrophysiology
laboratory, and a large echocardiographic laboratory were added
to Emory Hospital. New space also has been provided for a heart
failure service as well as a congenital heart disease clinic for
adults.
The Emory Heart Center was created in 1993. This new organization—including
the Andreas Gruentzig Cardiovascular Center at Emory Hospital, the
Carlyle Fraser Heart Center at Emory Crawford Long, and outpatient
cardiology with an outpatient cardiac catheterization laboratory
at The Emory Clinic—was designed to be the umbrella under
which clinical cardiology would thrive, fostering collaboration
and coordination among the many aspects of heart disease treatment
and diagnosis. Doug Morris, who is the J. Willis Hurst Professor
of Medicine, was chosen to be director of the Emory Heart Center.
The Heart Center has been ranked in the top 10 in the nation by
US News & World Report. In 2004, Emory’s program
in heart and heart surgery was ranked eighth–the only heart
program in Georgia included in the nation’s top 50.
These distinctions are well earned, and the first four years of
the new century continued to see growth in every area. The patient
care has become increasingly sophisticated and sought after. The
teaching programs for students, house officers, and fellows is increasingly
popular, and the research effort has achieved international recognition.
Taking stock in 2004 was rewarding because the audit of faculty
talent, space, and funds assures continued excellence in patient
care. Just look at a few examples. At Emory, patients routinely
can receive endoscopic cardiac bypass surgery, or hybrid coronary
revascularization, or high-tech cardiac resynchronization. Emory
patients likewise benefit from an ambitious research agenda, with
studies ranging from women’s cardiology to basic science.
For example, Peter Block, nationally known for his use of balloon
dilatation of the mitral valve for mitral stenosis, has recently
used the cardiac catheter to treat leakage of the mitral valve.
Active research efforts at the VAMC alone include cardiac ischemic
preconditioning, stem cell replacement therapy for cardiac injury,
and mechanical forces and atherosclerotic disease, to just name
a few. David Harrison, a superb researcher and clinician recognized
worldwide, is the Bernard Marcus Professor of Medicine and director
of the Division of Cardiology.
The Sibley Heart Center at Egleston opened in 2002, and 26 pediatric
cardiologists contribute to our pediatric cardiology efforts. Eleven
of these work at satellite locations throughout Georgia and are
members of the staff of 30 hospitals.
And the solidity of our programs continues at Emory Crawford Long
Hospital, where faculty members are using a biventricular pacemaker
to treat heart failure.
Emory can now boast of adequate research space for cardiology in
the enlarged Woodruff Research Building on the Emory campus, the
Atlanta VAMC, and at Emory Crawford Long. The funding of such a
large group of people comes from the money they earn from patients
they take care of in The Emory Clinic or in a similar facility,
from endowments, and from research grants. The annual research budget
from grants awarded to the Division of Cardiology alone is more
than $10 million.
Our teaching program remains strong. I’ll even go so far as
to say that the teaching program in cardiology for medical students
at Grady Memorial Hospital is one of the best in the nation. In
addition, all categorical interns and residents in general internal
medicine rotate through the cardiology service at Emory Hospital,
and the Emory cardiac fellowship program is one of the largest programs
in the country. A large number of cardiac fellows leave Emory to
populate the hospitals of Atlanta and other cities throughout the
nation and world. Many of them practice cardiology, and a significant
number joins academic research institutions. In fact, Emory has
trained 85% of practicing cardiologists and heart surgeons in Georgia.
From a fledgling effort in the 1940s, Emory cardiology has evolved
into the top 10 of the nation’s best heart centers. And that
is the story.
 I continue to teach
eight to 10 sessions in cardiology each week, and I write the remainder
of the time. Bruce Logue’s legacy is assured because the Georgia
affiliate of the American Heart Association has created an annual
dinner in which the R. Bruce Logue Excellence in Medicine award
is given to a worthy local physician. I join Logue, who is enjoying
his retirement, for lunch about once a month. We discuss the evolution
of Emory cardiology and smile. We remember when, in 1950, the two
of us were the only cardiologists in the entire Emory system and
there were only two cardiac surgeons. We smile because we both love
Emory and look with pleasure and awe at Emory cardiology today.
I continue to teach
eight to 10 sessions in cardiology each week, and I write the remainder
of the time. Bruce Logue’s legacy is assured because the Georgia
affiliate of the American Heart Association has created an annual
dinner in which the R. Bruce Logue Excellence in Medicine award
is given to a worthy local physician. I join Logue, who is enjoying
his retirement, for lunch about once a month. We discuss the evolution
of Emory cardiology and smile. We remember when, in 1950, the two
of us were the only cardiologists in the entire Emory system and
there were only two cardiac surgeons. We smile because we both love
Emory and look with pleasure and awe at Emory cardiology today. |
 |
| |
|
|
|
|
|





